An 89-year-old female presented to the emergency department with a three to four day history of gradually worsening, sharp right lower quadrant abdominal pain without radiation. On the day prior to the emergency room visit, a hard, tender mass developed in the area of discomfort. The patient usually had regular bowel movements; however she had not had a bowel movement for the past three days. The patient denied any fevers, nausea or vomiting associated with the abdominal pain. Review of systems was otherwise negative. Past medical history and past surgical history were not relevant to the current complaint.

Upon presentation to the emergency department, the patient was alert and in no acute distress. The patient’s vital signs were stable. Abdominal exam revealed decreased bowel sounds, tenderness in the right lower quadrant, guarding and rebound tenderness as well as a hard tender mass that was present in the right lower quadrant. The remainder of the physical exam was unremarkable. Pertinent laboratory data was all within normal range including the white blood cell count.

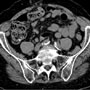
The initial impression was that the clinical picture depicted an incarcerated femoral hernia. However, a CT of the abdomen/pelvis without contrast was obtained which revealed a 3-4 cm nonspecific fluid collection in the right groin with indistinctness of fat surrounding and a hyperdensity within it that may reflect a dystrophic calcification. There were several lymph nodes adjacent to it as well (Image 1). With recommendation by the radiologist, an ultrasound of the right groin was obtained which revealed no signs of bowel in the mass, but possibly a hernia containing omental fat with fluid (Image 2). The radiologist also requested that a repeat CT of the abdomen / pelvis be obtained which reflected similar findings to the first CT (Image 3).
The patient was taken to surgery. Operative findings were those of an incarcerated appendix and omental fat within a femoral hernia. Therefore, it was not until surgical intervention that the diagnosis of De Garengeot’s Hernia was made. An appendectomy was then performed and subsequently a femoral hernia repair. The patient tolerated the procedure well and there were no post-surgical complications. The pathological report demonstrated an intact vermiform appendix that was of approximately normal size (5.8 cm in length with a diameter range of approximately 0.4 to 0.6) and vascular congestion evident with a distinctly hemorrhagic appearance. There were no inflammatory cells infiltrating the submucosa or other portions of the appendix typically found in acute appendicitis. There was yellow fibrofatty tissue, consistent with the initial radiologic description of omental fat attached to the appendix. The femoral hernia sac was also submitted for pathologic analysis. This appeared concave in shape and was pink and partially hemorrhagic.

De Garengeot’s hernia appears first in the literature as described by Jacques De Garengeot.1 It is rare, with only 242 reported cases in the literature as of 1974.2 The incidence has been previously described in the literature as approximately 1%.3,4 There is a slightly increased incidence described in female patients.5 No large case series have been published due to the low frequency of cases. However, a recent small case series found the presentation in 7 of 8 cases to be a painful groin lump. All 8 cases in the case series were diagnosed in the operating room upon intraoperative exploration of the hernia sac consistent with our case.4
Rarely, De Garengeot hernia’s have been effectively identified using radiologic evaluation. It has been described in the literature that CT evaluation has been the most sensitive modality for radiologic investigation of a suspicious femoral hernia.4 However, only a few cases of De Garengeot’s hernia have been effectively identified on CT scan prior to surgical exploration. 6,7 In retrospectively evaluating the CT in our case study, it was evident that the tubular structure within the hernia sac was an appendix. Fortunately, even if the diagnosis is made earlier with CT scan, the treatment for suspected incarcerated femoral hernias is emergent surgery.
The pathophysiology of De Garengeot’s femoral hernias has been long debated in the literature and there is no definitive conclusion. However, the majority of reported cases follow that the primary process is the initial entrapment of the appendix within the hernia sac which then can lead to subsequent inflammation, strangulation, necrosis or perforation. The alternative hypothesis is that the initial process is the inflammation of the appendix with entrapment in the hernia and subsequent potential for strangulation following as a secondarily.6 While, it is not possible to determine which pathophysiologic process preceded the other in our case, the resulting findings were evident on CT and later on pathologic specimen findings. Since the pathology report showed evidence of vascular congestion with hemorrhagic findings, we believe our case clinical findings are consistent with an incarcerated appendix within a femoral hernia.8
Finally, the surgical approach to these cases depends on the clinical presentation. Either an emergency laparotomy with or without an initial exploratory laparoscopy has been reported, although since an incarcerated femoral hernia was suspected in this case, a groin approach was used.4
Rare cases of De Garengeot’s hernia should be considered on the differential for patients presenting with right lower quadrant pain in the presence of what appears to be a groin mass consistent with the possibility of an incarcerated femoral hernia with bowel content. CT scan is helpful if the physician raises the index of suspicion for De Garengeot’s hernia given that the hernia sac contains a tubular mass with nearby fat stranding particularly when approximate to the cecum.
References
1. Akopian G, Alexander M. De Garengeot’s Hernia: appendicitis within a femoral hernia. Am Surg 2005; 71: 526-527.
2. Cordera F. Incarcerated Appendix in a Femoral Hernia Sac. Contemp Surg 2003; 59:35-37.
3. Tanner N. Strangulated Femoral Hernia Appendix with Perforated Sigmoid Diverticulitis. Proc R Soc Med 1963; 1105-1106.
4. Sharma H. De Garengeot Hernia: an analysis of our experience. Hernia 2007; 11:235-238.
5. Thomas B. De Garengeot Hernia. JSLS 2009; 13: 455-457.
6. D’Ambrosio N, Katz D, Hines J. Perforated Appendix within a Femoral Hernia. Journal of Roentgenology 2006; 186: 906-907.
7. Kagan A. De Garengeot’s Hernia: the importance of early diagnosis and its complications. Hernia online 2011. 1-3.
8. Pereira J, Sirlin C. Disproportionate Fat Stranding: A Helpful CT Sign in Patients with Acute Abdominal Pain. Radiographics 2004; 24:703-715.








3 Comments
I always remember the comical episode of Friends when Joey gets a hernia but can not afford treatment. Even though this is a funny episode having a hernia is no laughing matter. I am thankful that in England we do not have to pay for treatment so when my dad had an issue he could easily go for treatment of hernias in hertfordshire and he is no pain free!
I remember the episode where Ross, an adult mind you, goes to the same pediatrician he has seen his entire life and walks out with a lollipop.
I can totally relate.
I have an irrational phobia of anything medical, I’ve chosen not to leave certain places because I want to live in a proximity to where I can see the right doctor.
I’ve been overcharged for ultrasounds, bloodwork; had irrelevant medication pushed on me…my chosen PA now knows when I’ve been “non-compliant”, he’s monitoring my metabolism and most importantly- he’s HONEST and he keeps me comfortable.
I admit that I’m a total pain in the @$$ as a patient and the good doctors get a lot of credit from me. When I don’t feel good I can’t help it. It didn’t help when the gyno told me that the pain from endometriosis was “in my head”. Until I cleared most of it up. With Carnitine, choline/inositol.. I kid you not. I just take progesterone for cramps.
Oh btw, at some hospitals you can qualify for financial assistance and YES we do have medicare. It’s not wonderful but we have something.
Please note none of the 3 CT images on this page actually shows a right inguinal hernia.
It shows a fat containing hernia in the lower abdomen just to the right of midline.
Any chance of putting the relevant images on??
Sincerely,
E Tam (UK)