You are asked to see a stable multiple-trauma patient, 26 years old, who has fallen out of a tree (and you thought only kids climbed trees). He is intoxicated, and apparently fell striking his right side. The brunt of the fall was borne by the right arm, and he is unable to move his right elbow. He is complaining of severe pain. A screening head-to-toe trauma exam shows him to be alert &ox3, wearing a c-collar, and with some bruising of the right hip and thigh but no other findings. Vitals show only tachycardia. The right forearm is swollen just below the elbow, and the patient complains of severe pain with pronation/supination. Pulses and neuro function are intact distally.
A routine trauma evaluation is ordered, including CT of head-cspine-chest-abd-pelvis (the “Full Monty”). You order a portable chest and R elbow to include the proximal forearm, as well as the pelvis and R femur views. Pain meds are given, with good result.
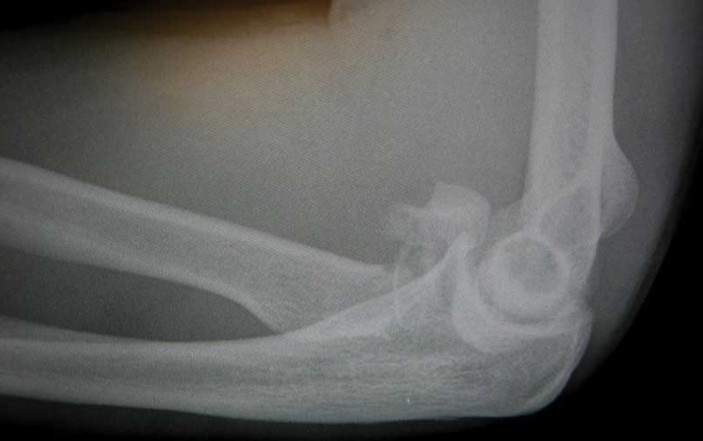
No surprise its broken – but this is an interesting fracture. We were expecting a Monteggia fracture, with a dislocated radial head and proximal ulna fracture. This fracture, which gave similar exam findings of pain, swelling and limited pronation/supination, is however a radial neck fracture with radial head dislocation. You can see the radial head pointing straight up (!) in dislocation. Radial neck fractures are usually seen in children (tree-climbers?) and have poor function outcome if resulting angulation exceeds 30-45 degrees.
This fracture is a Mason IIIb type fracture and can be managed adequately with only excision of the radial head. In one of the few follow-up studies published on this particular type of fracture in adult most patients reported no complaints after completely removing the dislocated radial head. Most reported a slight (less than 10 degree) loss of extension, and less than 5 degrees of lost flexion, forearm pronation, and supination.
Editor’s Note:
There are many nuances to fractures involving the elbow and their potential complications and definitive treatment options. Perhaps the most important issue facing EPs, however, is how to incorporate a diagnostic strategy into practice to avoid missing them. Does this mean that all patients with elbow trauma require radiographic evaluation? No. In fact, determining which patients need an X-ray and which do not is fairly easy. Range of motion and palpation are excellent predictors of elbow fracture. Appelboam, et al., in the British Medical Journal, 2008, reported that “elbow extension test” was very effective in predicting fractures in 958 adults and 778 pediatric patients. X-rays were ordered at the discretion of the physician in the pediatric group and only if the patient could not fully extend their elbow in the adult group. The test was 97.3% sensitive for elbow fractures in adults and 93.7% in children, while the negative predictive value was 96.5% and 93.7%, respectively. Two olecranon fractures were missed in the adult group. Thus, if palpation of the olecranon were included, the sensitivity would have improved. This suggests that palpation of the olecranon may also improve the sensitivity in the pediatric group despite the fact that no olecranon fractures were actually missed in the pediatric group. In summary, the ability to fully extend the elbow, in conjunction with the absence of olecranon tenderness, is a reasonable tool to incorporate into one’s practice to avoid missing elbow fractures, while reducing unnecessary X-rays.
Dr. Dallara practices Emergency Medicine in Virginia and North Carolina, and directs the Emergency Medicine PREP Course. www.emprepcourse.com