You are about to start your shift after a somewhat lengthy department meeting where one of the main topics discussed was utilization review with a special emphasis on cutting down the number of unnecessary advanced imaging studies. The physician champion for cutting down on unnecessary imaging had a lot of valid points. He stated that though advanced diagnostic imaging has many benefits, including first and foremost, decreased medical risk and, in general, better patient satisfaction, there are many down-sides, as well. Among these he listed were longer ED throughput times, unnecessary cost and having to explain and deal with the all too common incidental findings. The most important considerations, he opined, were exposure to the risks of ionizing radiation and of IV contrast associated with CT scanning.
After the meeting, the first patient you encounter is a 69-year-old man with a history of hypertension who presents with abdominal pain radiating to the back. He’s going to need a CT scan to rule out a AAA. Your second patient is a 23-year-old male who was hit in the head last night with a bottle and now has a splitting headache and recurrent vomiting. He’s going to need a CT scan too. You wonder if your third patient will require a CT as well? Will it be “three strikes and you’re out” or “third time’s a charm?” Great! As you pick up the chart, you see the chief complaint is “severe flank pain”.
The patient is a 25-year old female with a 2-hour history of severe left flank pain radiating to the groin. She states the pain came on suddenly and made her vomit twice. She denies missed periods, fever, dysuria and hematuria. She is otherwise healthy, but states her mom thinks it is a kidney stone because there is a family history of stones. You think to yourself that pyelo would be more likely given the demographics, but kidney stone, diverticulitis and pelvic pathology are also on your differential diagnosis radar. You’re at least thankful that the pain is not in the right lower quadrant.
You consider your approach. You’ll definitely need a UA and a pregnancy test. Will you need to do a CT scan? How about the dreaded pelvic exam? You decide to take to heart one of the strategies recommended at the end of the morning’s department meeting. One of your colleagues recommended forgoing formal imaging in patients with classic renal colic and no significant risk factors for aortic aneurysm or other more serious conditions as long as the UA was positive for blood. If you wanted additional diagnostic certainty, a focused ED sonogram could be done by the EP to look for hydronephrosis. You decide that this patient is perfect to implement this strategy on. She is young, so a AAA is pretty unlikely, and radiation from CT has the highest risk for younger patients.
You take the following image (image 1) of her left kidney. You also take a shot of her aorta to be safe and to practice your skills (image 2). What do the images show?
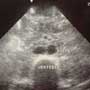
Image 1

Image 2

Should you take any other pictures? Do you need to do a formal imaging study
Dx: Mild Hydronephrosis
Image 1 shows the left kidney with mild hydronephrosis.

The renal parenchyma, outlined with asterisks, is echoic (dark gray), the renal pelvis is hyperechoic (white) and the dilated collecting system demonstrates mild hydronephrosis anechoic (black). No kidney stone is seen. Image 2 shows a cross section of her normal aorta, with the IVC and vertebral body labeled. Her aortic diameter is under 2cm. Time permitting, it is generally quite helpful to practice imaging other parts of the body. The ultrasound machine is already there and set up and the more you practice looking at normal anatomy, the better you will become at detecting abnormal findings.

Remember that it’s always a good idea to get a comparison view of structures that are bilateral. A view of a normal right kidney will help to ensure that the hydronephrosis on the painful side is indeed unilateral. If you see bilateral hydronephrosis with unilateral flank pain, you might need to expand your differential diagnosis a bit. Does your patient have distal obstruction? Are there two disease processes occurring simultaneously? Does that patient have an abscess, mass, or infarct that can’t be visualized well on bedside ultrasound?
As for the final question, “Do you need a formal study?” the answer is, “it depends.” How confident are you in your diagnosis and what was your pre-test probability? Are there red cells in the UA? Is the patient willing to wait or pay for additional testing? How backed up is the waiting room? Does your hospital or group have a policy covering this? Who is the patient going to follow-up with, and are they likely to applaud or complain about you? I can’t answer these questions for you, but I would be quite satisfied with myself if I saved her a CT scan.
Pearls & Pitfalls for Renal Ultrasound
1. Be Thorough: Image the entire organ by sweeping and fanning through the kidneys in two different planes. Don’t just go for one static shot through the middle and don’t stop scanning just because you visualize an abnormality. Always complete the entire scan so you don’t put yourself, and the patient, at risk for missing peripherally located pathology. If you have a difficult time imaging the left kidney, have the patient hold their breath to bring the kidney more caudally. Use the spleen and liver as your acoustic windows and don’t be afraid to reposition the patient to achieve better images. Any abnormal findings should be confirmed with comprehensive imaging via radiology, but this can often be done as an outpatient.
2. Look for Hydro: Hydronephrosis is seen as a black or anechoic area in the center of the kidney and represents downstream obstruction.
3. Compare Sides: Because most people have two kidneys, any questionable findings on one side may benefit from a comparison view of the other kidney.
4. Don’t Forget the Aorta: An aortic aneurysm often mimics renal colic, so always take a look at the aorta, even if your suspicion is low. It’s essential to practice looking at normal anatomy and even more essential to pick up an aneurysm before it ruptures.
5. Recognize Your Limitations: Remember that bedside ultrasound is meant to answer a specific, focused set of questions. It is not the same as a comprehensive, formal scan. You do not necessarily have to visualize the culprit stone if you see hydronephrosis. Likewise, it’s not always necessary to evaluate for ureteral jets within the bladder. Use the data an
d information you acquire from your beside scan to help guide management and treatment, but recognize that your scan is limited.
6. Take Responsibility for Your Findings: Document and archive all bedside ultrasound images and findings. If you find something incidental on your bedside scan, you are responsible for informing and educating the patient about the finding and advising or arranging appropriate follow-up.
7. Image in Urosepsis: Don’t miss renal obstruction in the setting of urosepsis as relieving the obstruction is a critical part of treatment. These patients may have little to no pain if they are elderly and/or the obstruction has become chronic. Be especially suspicious for obstruction if the patient does not have any other risk factor for UTI.
8. Practice Makes Perfect: With bedside ultrasound, there is no substitute for experience. The more ultrasounds you do, the better you will be able to differentiate abnormal from normal, even when you may not be sure exactly what the abnormality is. An image library of normal and abnormal ultrasounds helps immensely, and we can help. Just go to the ultrasound section on www.epmonthly.com.
RENAL STONES
A tip sheet from www.EMResource.org
Type: CaOxylate: 67%, TriplePhos: 12%, CaPhos: 8%, Cystine: 3%, Uric acid (radiolucent): 2%
Tests: UA: RBC:80-90%. KUB: 40-60% (1cm from spine). US: 65-95% (less if <6h). IVP: 87%
CT: 96%/98% (may miss uric acid, often due to Crixivan, but should detect hydronephrosis)
Passage: If < 2mm, 90% will pass w/in 4 days (up to 2wk).
Greater than 4mm, needs urology f/u.
8mm: Less than 10% pass.
Rx: Most pass w/in 2 weeks, lithotripsy (proximal stones <1cm), surgery, cystoscopy, (blocker
New: Nifedipine or Flowmax 0.4mg PO qd may lead to earlier passage. Steroids may help too.
Infection: Beware: fever, +UA, pH>7, staghorn stone, chronic obstruction (voided urine not sensitive)
Admit: Intractable pain or vomiting, hypercalcemia, solitary kidney,
Renal failure, high-grade obstruction, renal transplant, sepsis
Consider Admission: RI, stone>5mm, ruptured calyx, UTI (pH>7, >10 WBC/hpf on UA), urine extravasation
Risks: Dehydration, family history, Crohn’s, hypercalcemia, hyperthyroid, RTA, obesity (uric acid)
Meds: Crixivan (radiolucent stone), triamterene, sulfa…(See A to Z Pocket Pharmacopoeia for more)
DDx: PE, AAA (age>50), thrombosis/embolus (contrast CT to dx), diverticulitis, appy, pyelo
Papillary necrosis (NSAID, sickle cell), renal infarct, gynecologic conditions, CA
Copyright ERPocketBooks.com