It’s going to be one of those shifts. You just sent a 29- year-old male to the cardiac cath lab for a bona-fide ST elevation MI. Your patient with a chief complaint of “eye pain” ended up having metastatic cancer within his right orbit, and your seemingly straight-forward post-partum woman with a headache had an MR venogram showing a dural vein thrombosis. Although these are awesome teaching cases for your residents and medical students, you wonder out loud, “Where did the ankle sprains go?”
For your next case, your resident presents a 32-year-old male who drove himself to the ED because of right testicular pain. He notes the pain came on gradually over the past week, and it is “achy” and “heavy” in nature. On review of systems, he denies any fevers, chills, abdominal pain, dysuria, penile discharge, or recent trauma. He is sexually active with multiple partners, but has never had a sexually transmitted infection before. He notes he was on antibiotics recently for an “infected bug bite” on his arm, but is otherwise healthy and does not take any medications.
Other than being slightly tachycardic, the patient’s vital signs are within normal limits, and except for his testicles, the remainder of the physical examination is normal. Both testicles had a normal lie and there were no obvious external abnormalities. The epididymis felt normal bilaterally, but there was a rather odd palpable mass within the scrotal sac that your resident is concerned about. He wants you to help him figure out what it could be. For that matter, so does the patient.
Your astute resident rattles off his differential diagnosis for the patient’s testicular pain. He doesn’t think the patient has testicular torsion, torsion of the testicular appendage, epididymitis, orchitis, a hernia, or Fournier’s gangrene.
At the bedside, your stoic 32 year-old patient appears rather pleased that your resident is getting a “second opinion” and is happy his IV pain medications are finally kicking in. You take the opportunity to teach your resident about transillumination, the cremasteric reflex, and Prehn’s sign. On exam, you note that the right testicle does indeed feel more full along the inferior, posterior border. The area does not transilluminate, and it is definitely more tender to palpation than the surrounding tissue and contralateral testis.
Like a well-trained mind-reader, your resident excuses himself to grab the ED ultrasound machine, as you explain to the patient that you are going to do a focused bedside testicular scan to gather some more information about what could be going on.
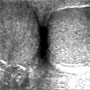
To begin your scan, you obtain a transverse image of both testicles side-by-side. By convention, the orientation marker is facing the patient’s right side (Top). What do you see? You zoom in on the abnormality and scan through the region of interest (B).


What should you be concerned about? Conclusion in the following
Dx: Calcified Lesion
You obtain a transverse image of both testicles to compare the echo-texture, size, and appearance of each testis. On the inferior and posterior aspect of the right testicle, you note a heterogeneous mass. Zooming in on the mass, you note a central hyperechoic, calcified lesion surrounded by hypoechoic fluid and peripheral edema.

The edges of the mass are indistinct and the mass is tender during your scan. Given the patient’s recent antibiotics, it could be a drug-resistant abscess, but it could also be a malignant testicular mass. You stand by as your resident explains to the patient that he is going to need a comprehensive ultrasound through the radiology department for further characterization of the mass, and that the plan is to touch base with Urology to determine the best management options available. The patient thanks you both for your care and asks if he can post his ultrasound images on Facebook.

As you and your resident walk the ultrasound machine back to its storage area, you can’t help but marvel at the pathology you have diagnosed and treated today.
“When you hear hoof-beats, you don’t always have to think zebras,” you tell your resident, “but remember that zebras do exist.”
“Zebras?!” the resident responds, “ With the way things have been going lately, I’m going to be on the lookout for a freakin’ unicorn!”
Pearls & Pitfalls for Bedside Testicular Ultrasound
1. It is often very difficult to determine the etiology of a patient’s testicular pain based on history and physical exam alone. When signs and symptoms overlap between various diagnoses, use ultrasound to obtain additional data.
2. A testicular scan is best performed with a high frequency, linear array transducer (10-5 MHz).
3. Have the patient lie supine with their knees bent and hips externally rotated to fully expose their testicles and scrotum. Place a rolled towel underneath their scrotum to help elevate it for better visualization and access during the scan.
4. Begin by obtaining a transverse view of both testes by placing the transducer underneath the testicles with the midline of the transducer centered along the scrotal raphe. Direct the beams in a cranial direction toward the patient’s head.
5. Scan through the unaffected testis first and obtain transverse images along the inferior, mid, and superior planes. Next, obtain longitudinal views along the medial, central, and lateral planes.
6. When scanning the painful or enlarged testis, compare its size and echogenicity to the contralateral side. A normal testis should measure approximately 3 cm wide and 5 cm long.
7. Obtain views of the epididymal head, body, and tail along the superior-posterior-lateral aspect of each testis.
8. If a palpable abnormality is encountered during the scan, obtain dedicated views of that region.
9. To improve your view of the entire organ, have the patient perform a Valsalva maneuver or “bear down” during the scan. Using warm ultrasound gel will also minimize the amount of testicular and scrotal retraction encountered during the scan.
10. Once the size and echogenicity of each testis has been evaluated, apply spectral or color/power Doppler to evaluate flow in each testis. Start with an image of both testes side-by-side and assess for symmetry of Doppler flow. Utilize low-flow detection settings and optimize transducer frequency to maximize Doppler sensitivity, meanwhile maintaining adequate penetration.
11. If flow cannot be easily v
isualized on color Doppler, use power Doppler over the area of concern. Spectral Doppler can be used to help determine if you are visualizing arterial or venous flow.
12. Suspicious masses or lesions require a comprehensive ultrasound and timely urologic follow-up. This patient ended up being diagnosed with testicular cancer and treatment has been initiated as an outpatient.