“I have to do a cost-benefit analysis of the situation,” your eager intern replies. It’s the end of the academic year and you are forcing your soon-to-be R2s to become more autonomous and confident in their management plans. You are amazed at the various answers you now get when you ask the simple question, “What do you want to do?”
You ask your intern to summarize the case for you. He just finished evaluating a 21-year-old male who presented to your ED with back pain. The patient states that his “back is killing him” and he thinks he strained his muscles working out too hard at the gym last week. He just started doing CrossFit and he’s worried that he overdid it. The patient notes that the pain is 10/10 and that he has had minimal relief with his friend’s Vicodin. He’s tried icing his back and even sat in the hot tub all weekend per his friend’s recommendation. Nothing is working so his friend told him to come into the ED to get a prescription for something “stronger.”
“Can’t wait to meet this friend…” you think to yourself. If only everything could be fixed with Vicodin and a hot tub. Your intern interrupts your thoughts as he continues to talk through the case out loud with you. His vital signs are normal except for some mild tachycardia at 105 bpm. The patient is otherwise healthy and has a good story for musculoskeletal strain. Your intern wants to give him a prescription for NSAID’s and recommendations for stretching, ice, and rest for the next week or so since his physical exam and history were “unremarkable” for any red flags.
Your question about whether or not this young 21 year old needs any imaging is giving him pause. “I think the cost of the imaging and the risk of radiation are too high. I don’t think there’s much benefit to keeping the patient here any longer. Plus I don’t know what we’d be looking for,” he replies. You are happy with your intern’s logic and pop into the room to see the patient. Within seconds, you realize that Vicodin and a hot tub probably won’t fix this patient’s pain. The patient is sitting hunched over on the stretcher rocking back and forth in pain. He has no appreciable tenderness to palpation over any of his back muscles, and there is no asymmetry or tightness on your exam. You are unable to reproduce or worsen his symptoms with testing his range of motion, but he is definitely rubbing his right lower back to try to ease his pain.
You walk out of the patient’s room and grab your intern and the ultrasound machine. As you head back towards the patient’s room, you pimp your intern on the other more serious causes of low back pain. Acknowledging that you have the ultrasound machine in tow, your clever intern starts rattling off the diagnoses that can be easily made with bedside ultrasound. AAA, atypical appendicitis, cholecystitis, nephrolithiasis, abscess, etc.
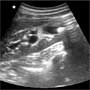
Since the patient is sitting upright and hunched over in pain, your intern decides to start his scan with a view of the right flank. What do you see on the bedside ultrasound? What’s the diagnosis? (Image 1).

What does the image show? Can you quickly and efficiently send the patient on his way home? Conclusion in the following

The patient’s bedside ultrasound reveals a large kidney stone with some surrounding hydronephrosis. The stone that you visualize is almost 10 mm in width and will likely need lithotripsy or interventional retrieval to help alleviate the patient’s pain (Image 2). As you wheel out the ultrasound machine, you overhear your intern telling the patient that a nurse will be in shortly to start an IV and provide the patient with intravenous analgesics. He finishes explaining the diagnosis and plan to the patient, and meets you at the computer station to finish his charting. You take a moment to finish your own note on the patient and look over to find a message taped to the chair next to you:
Cost of performing a quick bedside ultrasound:
- 5 minutes
- Cost of a bounce-back ED visit for a missed kidney stone: $3000
- Cost of a valuable lesson learned: priceless

Pearls & Pitfalls for PERFORMING Renal Ultra-sonography
01 Getting Started: Use the low frequency (5 to 1 MHz) phased array or curvilinear transducer. Remember that lower frequency transducers enable better visualization of deeper structures. Start with the right kidney, which is easier to find, by placing your probe in the coronal plane at the right flank. Use the liver as a window and obtain a view of the kidney in the long axis. You may need to tilt your probe in an oblique angle to get in between the ribs.
02 Be Thorough: Image the entire organ using a fanning motion. If you have a difficult time viewing either kidney, have the patient take a deep breath and then halt their inspiration. This brings both kidneys inferiorly. Obtain both long-axis and short-axis views of both kidneys.
03 Look for the Hydro: Hydronephrosis is seen as a black or anechoic area in the center of the kidney and usually represents downstream obstruction. Every so often, you may be able to visualize the culprit causing the obstruction. Large stones in the proximal ureter can be easily seen on ultrasound.
04 Compare Sides: Because most people have two kidneys, any questionable findings on one side may benefit from a comparison view of the other kidney. If your patient has bilateral hydronephrosis, always consider other causes besides kidney stones: bladder outlet obstruction, bladder cancer or intravesicular clots, valvular disease and reflux, or compression of the bilateral ureters by pregnancy, a mass, or intraperitoneal abnormalities.
05 Remember the Big Picture: During an emergency bedside ultrasound you don’t need to visualize the actual kidney stone or determine if there are ureteral jets into the bladder. The main focus of a bedside renal ultrasound is to determine if hydronephrosis is present. However, if there is a major abnormal finding, like it this case, take your time and get a good look at the sonographic abnormalities so that you are more likely to recognize abnormal scans when you see them.
06 Avoid Pitfalls: The best way to minimize errors is through experience, so scan lots of normal kidneys. With bedside ultrasound, there is no substitute for experience. The more scans you do, the better you will be able to differentiate abnormal from normal, even when you may not be sure exactly what the abnormality is. An image library of normal and abnormal ultrasounds helps immensely, and we can help. Just visit the Ultrasound section on EPMonthly.com.
07 Stay Current: Stay up to date on how you can use bedside ultrasound to enhance your clinical practice. Check out the ultrasound app “SonoSupport”. Available now for smartphones and tablets.









1 Comment
Am a fan of using ultrasound to help diagnose kidney stones and decrease CT scanning.
However I feel it should be pointed out that in the image above, the stone seen is not causing the person’s pain and does not necessarily require intervention. The location of the stone is in a pole of the kidney, not in a place where it would block the drainage system and cause symptoms. It does indicate the patient is a stone former, but the stone causing symptoms is likely somewhere along the ureter and not seen in this image. It may or may not be large enough to require intervention.
Chris Moore