During a busy swing shift, a 45-year-old male presents to the emergency department with two days of worsening right knee pain. He denies any injury, but states that the knee feels warm and swollen and now he can barely walk on it. He had a meniscal injury to the same knee about 8 years prior, and is now using crutches that he has left over from that time. He thinks he has gout because his brother and father have both had it with similar symptoms to his own. He denies any history of hardware in the knee, prior personal history of gout or joint infection, or any sexual exposures other than his wife of 15 years. His medical history is otherwise unremarkable and the only other surgery that he has had in the past was a splenectomy at age 18 from a motor vehicle accident.
On exam, he is an athletic male appearing younger than his stated age with a temperature of 99.4, blood pressure of 148/90, pulse of 83 and respiratory rate of 18. His head and neck exam are normal, as is his chest exam. His abdomen is non-tender with a well-healed left upper quadrant scar. The knee appears slightly swollen with a slightly reddish hue, but is not really warm. He can move it fairly decently while supine on the bed with some mild pain, but the area is fairly tender and he cannot bear weight on it.
Given the overall picture – his age, family history and the physical exam – you suspect new onset gout, but are worried that he could have a milder-than-usual presentation of a septic joint, especially since he has had prior surgery there and is minus a spleen. You therefore recommend a knee aspiration to be certain. “No way!” he answers. “I know those hurt and my brother has had those twice and they never even found any fluid. Can’t you just give me indomethacin and oxycodone like my brother gets? When he gets those, he is usually better in a few days.” You stick to your guns and answer, “Well then how do they even know that he really even has gout? The only way to tell for sure is to tap the joint. And what is more important, we need to make sure that you don’t have an infection in the knee, which would be dangerous to miss. The fact that you don’t have your spleen puts you at higher risk for infections, you know.”
Your patient appears to be pondering your words and weighing your arguments when you see his committed expression soften just a bit. He asks, “Doc, I don’t want to be a pain in the ass, and I certainly don’t want to have you give me medicine for gout if I really have an infection, but is there any way you can make sure there is fluid there so I don’t have to get stuck with a huge needle for no reason?” “Sure” you answer, “We can look at your knee with our ultrasound machine first to make sure there is a pocket of fluid to go after.” Knowing that ultrasound is more sensitive for a joint effusion than plain films, you decide to just skip the formal imaging and wheel over the department’s bedside ultrasound machine to take a peek (Image below).

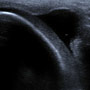
What do you see? What position do you think the knee was in for this image? Is there a fluid pocket? Conclusion in the following

Dx: Knee Effusion by Ultrasound
The image shows the distal femur with the knee in maximal tolerated flexion. With the knee in this position, fluid from within the joint is squeezed forward into a palpable bulge just lateral to the patellar tendon. On physical exam this is called the “Flex-Bulge sign” or “Pregerson sign” (yes I made it up, by examining my own knee I might add.) This bulge of fluid, which is easily palpated in the non-obese knee, especially when you compare to the contralateral side, is demonstrated on the ultrasound image as a semi-circle of hypoechoic fluid pocket. Flexion is probably the best position to use in order to pick up a small effusion. Knee flexion will often be limited in the presence of an effusion, so of course only do what is tolerable to the patient. Joint fluid, like most other fluid, appears black or anechoic and is clearly seen as a prominent anterior bulge in the ultrasound image. Of course this may also be easier to appreciate in a patient with an athletic build like this, rather than one who is soft and doughy.

You show the image to your patient, even giving him a comparison view using his other knee, to make sure he trusts you. He signs the consent form for the nurse, albeit somewhat apprehensively and you make sure to give him a nice dose of hydromorphone subcutaneously as well as generous local anesthesia, before proceeding with you arthrocentesis. Fortunately, when the results return they show negatively birefringent needle-shaped crystals and no bacteria. You tell your patient, “I’m glad to say that you were right! It looks like gout. I’ll send you home with those prescriptions you requested, but if it gets any worse, or you get a fever, return immediately.” He answers with a smile, “You were right too doc. It’s better to be safe than sorry.”

Tips & Tricks for the Ultrasound Evaluation of a Joint Effusion
01 Look before You Leap: Ultrasound can be used to help you delineate whether a patient has a joint effusion or not. It is more sensitive than x-ray and can also help you localize the best area to tap. It may be prudent to perform a bedside ultrasound prior to an arthrocentesis attempt when physical exam findings are equivocal.
02 Go Linear: For most joints use a 5 to 7.5 MHz linear array transducer. Apply a large amount of ultrasound gel to improve your acoustic interface. If the patient is thin and devoid of much subcutaneous fat, you may need to utilize an acoustic standoff pad or water submersion to improve your sonographic window.
03 Take Multiple Views: Always obtain images in multiple planes (longitudinal, transverse, oblique) to help define the borders of the structure you are looking at and avoid mistaking vascular structures for a joint effusion. Apply color or spectral Doppler if there is any concern that you may be looking at a vascular structure. Use ultrasound to find the best and largest fluid pocket to tap.
04 Compare Sides: Utilize contra-lateral limbs for comparison views, especially when unsure of what you see. If you see a similar structure on the asymptomatic limb, you may need to look again.
05 Don’t Move: Avoid changing the position of the joint between performing the bedside ultrasound and performing the arthrocentesis. Fluid may move with joint repositioning. If you decide to perform a dynamic
ultrasound-guided joint aspiration, make sure you prep and drape the probe in a sterile fashion prior to beginning your procedure.