The labs have all come back on a 38-year-old female who you suspected had pyelonephritis. She had presented with 24 hours of flank pain and fever but no vomiting, abdominal pain or dysuria. Her last menstrual period was 2 weeks ago and she denies any possibility of pregnancy. Her past medical history was only significant for hypertension treated with hydrochlorothiazide. Her physical exam showed no surprises: She was afebrile despite the history of fever at home, and she was slightly hypertensive with a BP of 157/93 mmHg. Other than right costo-vertebral angle tenderness, the rest of her exam was normal.
Her labs unfortunately are giving you a few uncomfortable surprises. Her CBC shows an expected leukocytosis with a WBC count of 14.9, but the rest of the values are normal. The unexpected twists are her abnormal renal function and the amount of blood in her urine. Her creatinine is 2.4. She is unaware of any prior kidney damage, but doesn’t know when she last had blood tests. The rest of her chemistry panel is normal except for a potassium of 3.2 and a bicarb or 34, both of which you attribute to her hydrochlorothiazide. She does have old labs on file, which are normal, but they are from 2001. She states that she has been on blood pressure medication for about 5 years. You wonder if it is the hypertension alone that has started to cook her beans.
Her UA has some remarkable abnormalities, as well. There are only 5-10 WBC’s per high powered field (hpf) and 2+ bacteria, but >200 RBC’s per hpf. You’ve diagnosed many cases of pyelonephritis with only 5-10 WBC’s per hpf, some with even fewer, especially when there is bacteruria. Despite unimpressive pyuria, when you’ve checked the urine cultures a few days later, they often came back positive when your clinical suspicion was otherwise high, and even some times when it wasn’t. And, since bacteruria is 90-95% specific for a UTI, you feel pretty confident that your patient today does indeed have pyelonephritis with only 5-10 WBC’s to show for it. What is bothering you about the UA is actually the number of RBC’s. In hemorrhagic cystitis you can certainly get lots of RBC’s and even have more RBC’s than WBC’s, but this patient does not have dysuria. She’s mid-cycle and denies any vaginal bleeding, so that’s not the explanation. You are worried that she may have a concomitant kidney stone and so some type of imaging will be necessary.
Since she is relatively young, you especially want to avoid unnecessary radiation so you would prefer to get an ultrasound. However, you know that CT is more sensitive and this is one of the few cases where you really wouldn’t want to miss a kidney stone, because concomitant infection is one of the few exceptions to the rule, “No one ever died from a kidney stone”. You decide that you will use the ED portable ultrasound machine to take a quick look. If you see hydronephrosis, so will the radiologist, and so you’ll order the ultrasound and spare your patient the radiation. If the kidneys look normal, however, you’ll order the more definitive CT-urogram.
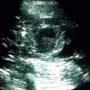
You wheel over one of your department’s machines and get the image above. Is there hydronephrosis? Conclusion in the following
Dx: Renal Cyst
 Your sonogram shows not hydronephrosis, but instead a renal cyst. And it’s not even a simple cyst, but rather an infected cyst that has internal echoes causing a hypoechoic (dark gray), rather than an anechoic (black) center on its lower half. To the neophyte sonographer, a cyst might be mistaken for hydronephrosis caused by a kidney stone. Cysts, however, can be distinguished by both their shape and location; they tend to be both more peripheral and more circular. This patient actually had other cysts and an abnormal renal parenchyma, which made the boundaries of kidney somewhat difficult to identify. She later underwent a comprehensive ultrasound in the radiology department, which diagnosed polycystic kidney disease complicated by an infected cyst. She was continued on antibiotics during her 3 day hospitalization and on day 2 had a CT-guided drainage of the infected cyst. Though you did your best to avoid radiation exposure in the ED, your colleagues upstairs did not continue in the same spirit. Her CT with contrast is shown, in addition to an image from her comprehensive ultrasound.
Your sonogram shows not hydronephrosis, but instead a renal cyst. And it’s not even a simple cyst, but rather an infected cyst that has internal echoes causing a hypoechoic (dark gray), rather than an anechoic (black) center on its lower half. To the neophyte sonographer, a cyst might be mistaken for hydronephrosis caused by a kidney stone. Cysts, however, can be distinguished by both their shape and location; they tend to be both more peripheral and more circular. This patient actually had other cysts and an abnormal renal parenchyma, which made the boundaries of kidney somewhat difficult to identify. She later underwent a comprehensive ultrasound in the radiology department, which diagnosed polycystic kidney disease complicated by an infected cyst. She was continued on antibiotics during her 3 day hospitalization and on day 2 had a CT-guided drainage of the infected cyst. Though you did your best to avoid radiation exposure in the ED, your colleagues upstairs did not continue in the same spirit. Her CT with contrast is shown, in addition to an image from her comprehensive ultrasound.
 You are glad you decided to take your evaluation one step further than you normally do for what at first appeared to be routine pyelonephritis. Remember, when things don’t seem to fit, it’s wise to look further and consider a broader differential. In this case the rule, “If red cells exceed white cells in the urine for a patient who clinically has pyelonephritis, look for another cause” was the one that started the search that eventually led to a diagnosis of polycystic kidney disease which explained both the patient’s elevated creatinine and her hematuria. Had this diagnosis been missed, antibiotic therapy alone would have likely been ineffective. Definitive management required drainage of the infected cyst.
You are glad you decided to take your evaluation one step further than you normally do for what at first appeared to be routine pyelonephritis. Remember, when things don’t seem to fit, it’s wise to look further and consider a broader differential. In this case the rule, “If red cells exceed white cells in the urine for a patient who clinically has pyelonephritis, look for another cause” was the one that started the search that eventually led to a diagnosis of polycystic kidney disease which explained both the patient’s elevated creatinine and her hematuria. Had this diagnosis been missed, antibiotic therapy alone would have likely been ineffective. Definitive management required drainage of the infected cyst.
 However, when things do fit together well, you don’t always need advanced imaging to care for patients with headache, chest pain, flank pain or abdominal pain. Renal colic is a perfect example of where we can cut down the use of unnecessary CT scanning. CT adds significant radiation exposure, not to mention cost as well as delays for other patients. When you are worried about more serious causes of flank pain, such as a AAA, image liberally, but since for the most part, kidney stones can be treated expectantly and most stones will pass on their own, it makes little sense to CT most young, healthy, afebrile patients with flank pain and blood in their urine, especially if they’ve had a kidney stone in the past. If you are uncomfortable with no imaging, at least consider ultrasound, as it is radiation free.
However, when things do fit together well, you don’t always need advanced imaging to care for patients with headache, chest pain, flank pain or abdominal pain. Renal colic is a perfect example of where we can cut down the use of unnecessary CT scanning. CT adds significant radiation exposure, not to mention cost as well as delays for other patients. When you are worried about more serious causes of flank pain, such as a AAA, image liberally, but since for the most part, kidney stones can be treated expectantly and most stones will pass on their own, it makes little sense to CT most young, healthy, afebrile patients with flank pain and blood in their urine, especially if they’ve had a kidney stone in the past. If you are uncomfortable with no imaging, at least consider ultrasound, as it is radiation free.
Minimizing radiation exposure is an important part of patient care. Though more testing tends to be in our best interest as providers, it is often not in our patients’ best interest. We all took an oath in medical school that included a phrase promising to put our patient’s well-being before our own. Let’s make good on that oath. Fo
r more information on radiation stewardship and radiation doses from various tests, visit the Image Gently campaign at www.pedrad.org and also the Radiation Stewardship page on www.erpocketbooks.com.
Pearls & Pitfalls for Renal Ultrasonography
1. What probes can you use? Typically, the kidneys are best visualized using a 5-2 MHz curvilinear probe or a 5-1 MHz phased array transducer. The smaller footprint of the phased array transducer enables the operator to maneuver the face of the probe in between the patient’s ribs.
2. Be Thorough: Image the entire organ using a fanning motion. Don’t just go for one isolated static shot through the middle of the kidney. Obtain complete views of the kidneys in both the longitudinal and transverse fashion. If you have a difficult time imaging the left kidney, have the patient hold their breath to bring the kidney more inferiorly. Use the spleen as your acoustic window on the left and the liver as your acoustic window on the right. Slide your transducer in an oblique angle in between the ribs to minimize the amount of rib shadowing obstructing your view of the kidney. Any abnormal findings should be confirmed with comprehensive imaging via radiology, but this can often be done as an outpatient.
3. Look for Hydro: Hydronephrosis is seen as a black or anechoic area in the center of the kidney and represents downstream obstruction. Shape is often irregular and varies depending on severity. Hydronephrosis can be categorized as mild, moderate, or severe. Cysts tend to be circular and more peripherally located than hydronephrosis.
4. Compare Sides: Because most people have two kidneys, any questionable findings on one side may benefit from a comparison view of the other kidney. If bilateral hydronephrosis is detected, image the urinary bladder to ensure there is no bladder retention or downstream obstruction.
5. Don’t Forget the Aorta: An aortic aneurysm often mimics renal colic. So always take a look at the aorta, even if your suspicion is low. It’s essential to practice looking at normal anatomy and even more essential to pick up an aneurysm before it ruptures.
6. Don’t Worry about Details: During an ED ultrasound it’s not necessarily your job to find the stone itself or to look for ureteral jets into the bladder. Concentrate on looking for hydronephrosis. Note that often times, stones may not be seen on bedside ultrasound, but their acoustic shadows may be picked up during your scan through the kidney and proximal ureter.
7. Image in Urosepsis: Don’t miss renal obstruction in the setting of urosepsis. Remember that relieving the obstruction is a critical part of treatment. These patients may have little to no pain if they are elderly and/or the obstruction has become chronic. Be especially suspicious for obstruction if the patient does not have any other risk factors for a UTI.
8. Practice: With bedside ultrasound, there is no substitute for experience. The more scans you do, the better you will be able to differentiate abnormal from normal, even when you may not be sure exactly what the abnormality is. An image library of normal and abnormal ultrasounds helps immensely, and we can help. Just go to the Soundings department on www.epmonthly.com.