You got stuck with another holiday shift. As usual it starts off slow, but eventually a bolus of patients arrives, to make up for lost time and then some. Fortunately most of your patients aren’t that sick. Many are visiting from out of town and staying with family. Some forgot their medications on the other side of the country and so their blood pressure or chronic pain or – fill in the blank – is out of control. Some would have seen their regular doctor for their admittedly minor issue, but alas, it is the holidays and everything is closed or booked. As you sort through tonight’s patients – and their emptied rooms are all too quickly refilled – you eventually meet someone who actually, desperately, needs your help.
He is a lethargic and slightly hypotensive 38-year-old male with a history of diabetes, hypertension, hepatitis C, cirrhosis and methamphetamine abuse who is brought in by family for trouble breathing and weakness that has progressively worsened over the past 24 hours. Though he doesn’t give much history himself, his family states he had been complaining of some chest pain as well. There has been no fever, vomiting, diarrhea, cough or other problems, and he has never had this constellation of symptoms before.
On exam you note that he is somewhat lethargic, answering questions with little more than a yes or a no. His vital signs are all normal except for his blood pressure, which is 83/41 mmHg. Though he is short of breath, his pulse ox is actually normal at 98% on room air. His head and neck exam is remarkable for somewhat dry mucosa coupled oddly enough with a bit of JVD. His lungs sound clear, but he is slightly tachypneic. His heart has a noticeable systolic ejection murmur which is new per family, although they admit they can’t be completely certain. His abdomen is non-tender and he has no appreciable peripheral edema.
Testing shows diffuse anterior ST depression on EKG, and cardiomegaly without infiltrates on chest X-ray. His white blood cell count is elevated at 15, his troponin and creatinine are both 2.3, his BNP is 540 and his lactate level is 5.5. The rest of his chemistries and other lab tests show more abnormals than normals. Seeing that you are obviously dealing with a sick patient you get on the phone with the hospitalist to admit the patient to the ICU and the cardiologist to see if he wants to take the patient to the cath lab or approve a stat echocardiogram. Unfortunately, it’s late at night and it’s also a holiday.
The cardiologist recommends cautious fluid resuscitation and pressors if necessary. They can do an echocardiogram early the next morning. You feel a bit uncomfortable with the recommendations as you are not sure what is causing this patient’s hypotension and you worry about a cardiac cause since there is a new murmur on exam. However, it is late and your consultant is the chief of cardiology, and most importantly he has a number of recommendations which are sound. This could after all be sepsis, or a PE or dehydration or something else. And even if it is cardiac, there is no ST-elevation and no one is going to come do an emergent valve repair in a patient in the middle of the night, especially if you haven’t even really done much yet to try to stabilize him medically.
You decide not to fight this battle, and take care of this patient the best you can without having the echo tech called in for a stat afterhours study. Then you graciously thank your consultant, hang up the phone and fire up the ED ultrasound machine to take a look yourself.
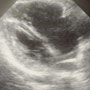
What various conditions should you be looking for and what would they look like on bedside ultrasound? Of these, which is seen on the parasternal view of the heart below?
Dx: Acute Pulmonary Hypertension
 PULMONARY HYPERTENSION
PULMONARY HYPERTENSION
from Quick Essentials Emergency Medicine 4.0, EMresource.org
Clinical: Dyspnea, chest pain, angina, syncope. Narrow split S2, RV hypertrophy, right sided CHF.
Tests: CXR: large pulmonary artery. Echo: dilated RV & pulmonary artery
Causes: Hypoxia, chronic lung dz, drugs, cirrhosis, chronic PE’s, scleroderma/SLE, cardiac shunt
Drugs: Methamphetamine, cocaine, Fen-phen
Rx-chronic: O2, fix pH, prostacycline, dig, Revatio, Bosentan, Coumadin, nifedipine, lung transplant
Rx-acute: Diuresis, phlebotomy, thrombectomy, pressors. Avoid intubation & overly aggressive fluidz
*****************
There are a number of conditions you should be looking for in the setting of shock. A bedside ultrasound scan can help you narrow down your differential: pericardial tamponade, PE, MI, hypovolemia, aortic dissection, and ruptured AAA are some at the top of the list. Since there is not room to show all of these here, you may want to check out the free ultrasound image library at www.erpocketbooks.com as you read on.
With cardiomegaly on the chest X-ray, especially if you don’t know that it’s chronic, your first consideration should be cardiac tamponade from a large pericardial effusion. A bedside echo should be able to rule this out quite easily. On a quick look, your patient does not have any signs of an effusion, so you move on. Given the heart murmur, your next consideration should probably be cardiogenic shock, and if this were the case you would expect to see a dilated, hypokinetic left ventricle (LV). However the LV is actually small and it is the right ventricle (RV) that appears enlarged. This should make you suspect a pulmonary embolism, however this was eventually ruled out with a pulmonary angiogram. As it turned out this patient was eventually diagnosed with acute pulmonary hypertension, possibly due to a combination or cirrhosis and methamphetamine abuse (see above for facts on pulmonary hypertension).
Other conditions that the ultrasound machine could be helpful with include hypovolemic shock, where you would expect to see a small rapidly beating heart and a shrunken or flat inferior vena cava. If you look carefully in the right patient, it is possible to pick up an intimal flap from an acute aortic dissection. Imaging the belly for an abdominal aortic aneurysm or free fluid from a ruptured spleen or hemorrhagic pancreatitis might also be helpful in narrowing down the cause of shock in a sick patient. In the setting of a new murmur, valvular pathology or an acute MI should also be considerations. Imaging for these conditions however, is beyond the scope of most emergency physicians, so when you are worried about these a formal echocardiogram is desirable.
Pearls & Pitfalls for Ultrasound of Hypotensive Patients
1. Start with the heart. Parasternal ima
ges tend to give the most information, but the subxyphoid view may be easier in some patients. Look for effusions, chamber dilation, and wall motion abnormalities (advanced).
2. Use the curvilinear probe or the phased array transducer. Start in the 4th intercostal space and position the probe between the ribs. If you do not get a good image try moving up or down one rib space and redirecting the angle of your probe. Remember to direct the beams of your probe through the long axis of the heart. If you need to decrease the distance between the patient’s heart and the ultrasound beams, have the patient roll over onto their left side and bring their heart closer to their chest wall.
3. Take the time to adjust your depth and gain to maximize image quality. Make sure you have enough depth to look behind the heart for a pericardial effusion. You should always try to see the cross-sectional descending aorta coursing behind the left ventricle.
4. In the setting of hypotension, pericardial fluid, especially when accompanied by right ventricular collapse, may signify tamponade, a condition which is best treated by immediate pericardiocentesis. Pleural effusions may mimic pericardial effusions in certain instances. If you are unsure, find the retrocardiac aorta. If the fluid is between the heart and aorta, it is pericardial. If it is on the opposite side of the aorta from the heart, it is pleural.
5. A hyperdynamic rapidly beating heart usually signifies hypovolemia. Look at the IVC to assess if the patient is indeed intravascularly depleted. Many studies have correlated IVC diameter to Swan Ganz RA pressures. If the heart is hyperdynamic and the IVC is compressed, the aggressive administration of fluids or blood products may be life-saving. Consider a search for the source of bleeding. Look for melena, hemoperitoneum, or an aortic aneurysm.
6. A dilated right ventricle should raise your suspicion for a massive pulmonary embolism. In such cases, tPA should be considered. Remember that CHF or pulmonary hypertension can also cause a dilated RV, although these chronic conditions will show a dilated RV with hypertrophy of the RV walls. A dilated RV with thin walls prompt consideration of the diagnosis of an acute massive PE.
7. Scanning further south may also help find the cause. Image the abdomen for evidence of retro-peritoneal bleeding from a ruptured AAA, or intraperitoneal bleeding from occult trauma, or ruptured ectopic pregnancy or spleen. Ultrasound of the legs may show DVT.
8. Ultrasound may be useful for more than just establishing a diagnosis. It can also help with procedures such as central line placement and pericardiocentesis during the resuscitation.
9. Consider the CORE Scan (Concentrated Overview of Resuscitative Efforts) in all undifferentiated hypotensive patients: https://apps.acep.org/WorkArea/DownloadAsset.aspx?id=42470