Your next ED patient is a 47 year old male with a history of diabetes, hypertension, coronary arterial disease and CHF who presents with 2 weeks of gradually worsening leg swelling, abdominal swelling, and trouble sleeping due to orthopnea. He states that he has had the leg swelling and trouble breathing in the past from his CHF, but he has never had a “jelly belly” before. He denies any change in his medications or dietary indiscretion. He has not had any chest pain, abdominal pain other than feeling “fat and bloated” or any vomiting, diarrhea or fever. His main concern seems to be his abdomen and his request is simple. “Doc, can you fix me?”
Your next ED patient is a 47 year old male with a history of diabetes, hypertension, coronary arterial disease and CHF who presents with 2 weeks of gradually worsening leg swelling, abdominal swelling, and trouble sleeping due to orthopnea. He states that he has had the leg swelling and trouble breathing in the past from his CHF, but he has never had a “jelly belly” before. He denies any change in his medications or dietary indiscretion. He has not had any chest pain, abdominal pain other than feeling “fat and bloated” or any vomiting, diarrhea or fever. His main concern seems to be his abdomen and his request is simple. “Doc, can you fix me?”
On physical exam, he is in no acute distress but is a bit hypertensive and tachypneic. His temperature is 96.8°F with a respiratory rate of 24 and a pulse ox of 96% on room air. His pulse and blood pressure are 68 and 179/96, respectively. His head and neck appear normal except for his eyes, which have just the slightest tint of yellow. His lungs are clear, but he has decreased breath sounds bilaterally. His heart is regular, without murmur or gallop. His abdomen is quite distended, but non-tender, and he has a positive fluid wave. His extremities have symmetric 2+ edema, without redness or tenderness.
You order some basic tests and none of the results surprise you much. His EKG and chest X-ray show nothing acute, just poor inspiration. His potassium is a bit low and his bicarb a bit high from the Lasix he is taking, but otherwise his metabolic panel looks good. His CBC is fine except for low platelets at 111,000. His troponin is normal, but his BNP and LFT’s are all slightly out of whack.
You call his internist to admit him for a mild CHF exacerbation with new onset ascites, likely due to a combination of the CHF and previously undiagnosed liver disease. His internist agrees, but wants you to tap his abdomen first – conditions, conditions.
“This guy is breathing fine,” you think to yourself. “He doesn’t really need the tap done now, and the ED is pretty busy. I don’t really want to give myself more work, but it is Saturday evening, and if I don’t do it, it probably won’t be done till midday on Monday.”
You tell the internist, “sure,” then, after getting off the phone, you ask one of your trusty ED techs to set you up for a paracentesis. As an afterthought you add, “Better get the ultrasound machine in there as well.” You might as well confirm 100% that there is actually fluid in there, that there is enough to tap, and where the safest puncture location is.
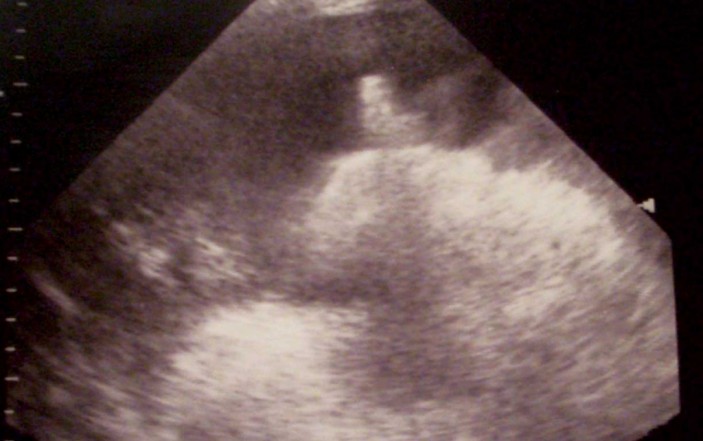
When the time is ripe, you turn on your ultrasound machine, add a small dab of gel to the curvilinear probe and take the following image (below) in the right lower quadrant.
What do you see? Is there ascites?
If so, how much? Does this look like a promising location or should you look elsewhere?
Would repositioning your patient help?
Factors other than pocket size are important to consider as well. For example, you want to avoid puncturing an enlarged liver or spleen. Find adjacent organs while you are performing your scan. You also would want to avoid any surgical scars, because adhesions in the area may tether down bowel and increase the risk that you will perforate them with your needle. Proper positioning for paracentesis is also important. Since bowel floats, it is recommended that the patient be positioned with the head of the bed elevated between 45 and 60 degrees. The bowel will rise and the fluid will collect in the lower abdomen. Repositioning the patient after the ultrasound, but before the tap however, is ill advised. Any repositioning may cause the bowel and fluid to shift and increases the risk of hitting bowel. The one botched tap I have done was due to repositioning a patient. He had a belly full of fluid by an ultrasound that was done in the supine position. I then sat him up to do the tap and could not get any fluid at all. I ended up aspirating peritoneal gas. When I ultrasounded him again, all the fluid had mysteriously disappeared. As it turned out, the patient’s “ascitic fluid” was actually all urine due to a ruptured bladder, and when I had repositioned him, it had all siphoned off into the Foley catheter that the nurse had placed. This scenario is rare, but it reinforces the importance of doing the ultrasound right before you do the tap, with no repositioning in between.
PARACENTESIS: (Safest with real time US guidance)
Indications
-Diagnostic: new ascites, r/o infected ascites
-Therapeutic: tense ascites, respiratory distress
Contraindications:
-Uncooperative patient, scar or cellulitis at site, bowel
obstruction, pregnant, DIC, tPA in use
Relative: INR >1.5-5.0
-Most experts say tap is OK regardless of INR.
-Platelets < 50. Attempts to correct INR may cause more complications than the procedure itself.
Preparation:
-Decompress bladder, position HOB at 45-60° (bowel floats) then use US to find best pocket
-Use curved probe. Find and measure biggest fluid pocket (usually RLQ or LLQ) with no vessels or organs in way.
-Don’t reposition patient after ultrasound, as fluid may move. Avoid scars, veins & big spleen
-Use Z-puncture. Pull skin down 2 cm before inserting needle to prevent leakage from site afterwards
Diagnosis:
-SBP: > 250 PMNs, >1000 WBC, Serum-Ascitic Albumin Gradient < 1.1
-Exudative: Protein >3 or ratio >0.5. LDH >200 or ratio >0.6, specific gravity >1.016
3. Do the Tap: Most practitioners will localize a fluid pocket with ultrasound and then complete the procedure in a “blind” fashion. You can use ultrasound to localize the best fluid pocket and then mark the puncture site with a marker before you prep and drape the patient. Alternatively, you can prep your probe in a sterile fashion and complete the procedure with real-time ultrasound guidance. If you choose the latter, you may want to have an assistant hold the ultrasound probe for you so that you have use of both of your hands.
4. Practice Makes Perfect: With bedside ultrasound, there is no substitute for experience. The more ultrasounds you do, the better you will be able to differentiate abnormal from normal, even when you may not be sure exactly what the abnormality is. An image library of normal and abnormal ultrasounds helps immensely, and EPM can help. Just go to EPMonthly.com and click the ultrasound library link within the Real-Time-Readings department.
5. Caution should be taken removing too much fluid too quickly. Some patients with as little as 1.5 L removed too quickly have experienced hypotension.