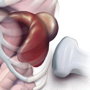
They say that things come in threes, and at least for today, you agree. You just finished sending home three young women with first trimester vaginal bleeding and reassuring bedside ultrasounds. Prior to that you actually had three cardiac arrests, one that you remarkably brought back with tPA after your bedside echo showed a severely dilated right ventricle but normal left ventricle from a presumed acute PE. Now you are onto your triad of abdominal pains for the day. The first two have been relatively simple. You admitted your patient with pancreatitis and intractable nausea and vomiting, and you’ve discharged your young lady with gastritis from the new NSAID she’s been taking for her meniscus injury. Your last abdominal pain patient is giving you slight pause. Fortunately, or unfortunately, his workup has been negative thus far: normal labs and no response to your favorite “white warrior” cocktail (Maalox and lidocaine). Other than tachycardia, his vital signs have been normal and his serial exams have not revealed any new clues. Typically, you would just send a patient like this home without imaging since it will probably be low yield, but something about this guy just isn’t right. He looked truly uncomfortable on presentation and has now required a second milligram of Dilaudid to get his pain under control despite being narcotic naïve. You suspect that something is going on but don’t really feel an emergency CT scan is warranted due to both the radiation risks and the log-jam that is developing in your department’s waiting room. You decide to brandish your trusty sword to dispense with this dilemma. You roll in with your ultrasound machine and unsheathe the ultrasound probe. While applying a cherry-sized dab of gel to the business end you proclaim, “Let’s take a look inside you” to your patient. You take a few cuts of the left kidney and left lung fields, but see no hydronephrosis, renal cysts, stones, or pulmonary abnormalities. Slashing through the heart and stomach, you visualize a normal heart and note that the stomach is not enlarged. You pierce your beams towards the pancreas and all appears well. You next aim at the aorta, and it appears normal, too. Finally you swashbuckle your way to the spleen and obtain the following view (Image 1).
What does your ultrasound show? Your waiting room continues to swell—what should you do next?

Left Upper Quadrant Pain
 Image 1 was taken with the curvilinear probe in a longitudinal fashion in the left anterior axillary line at around T8. Compare this to a normal left upper quadrant view of the splenorenal interface in Image 3. Your patient has a large splenic cyst that measures about 7.5 cm in width (Image 2). The cyst has an anechoic center with a thin wall nearfield and a brighter/whiter wall farfield on the screen. Note the bright white enhancement of the posterior medial wall of the cyst. This echogenic artifact make it look like the diaphragm is wrapping around the medial aspect of the cyst. You are surprised at your ultrasound findings since it is quite rare to find cysts in the spleen. You remember reading that they can occur following trauma, with echinococcal infections, from congenital or metastatic etiologies, and sometimes with polycystic kidney disease. As there were no cysts seen in the adjacent kidney, you think PCKD is unlikely. He denies any recent travel or trauma, and his family history in unremarkable for any cysts or other concerning diseases. Given that you have ruled-out the emergent causes of this guy’s pain with your labs, bedside ultrasound, and serial exams in the ED, you decide that this cyst is likely the cause of your patient’s pain. Your waiting room isn’t emptying out so you decide to call the patient’s PCP and arrange follow-up and outpatient comprehensive imaging.
Image 1 was taken with the curvilinear probe in a longitudinal fashion in the left anterior axillary line at around T8. Compare this to a normal left upper quadrant view of the splenorenal interface in Image 3. Your patient has a large splenic cyst that measures about 7.5 cm in width (Image 2). The cyst has an anechoic center with a thin wall nearfield and a brighter/whiter wall farfield on the screen. Note the bright white enhancement of the posterior medial wall of the cyst. This echogenic artifact make it look like the diaphragm is wrapping around the medial aspect of the cyst. You are surprised at your ultrasound findings since it is quite rare to find cysts in the spleen. You remember reading that they can occur following trauma, with echinococcal infections, from congenital or metastatic etiologies, and sometimes with polycystic kidney disease. As there were no cysts seen in the adjacent kidney, you think PCKD is unlikely. He denies any recent travel or trauma, and his family history in unremarkable for any cysts or other concerning diseases. Given that you have ruled-out the emergent causes of this guy’s pain with your labs, bedside ultrasound, and serial exams in the ED, you decide that this cyst is likely the cause of your patient’s pain. Your waiting room isn’t emptying out so you decide to call the patient’s PCP and arrange follow-up and outpatient comprehensive imaging.
Three weeks later the patient is doing well using over the counter analgesics. His follow-up ultrasound showed that the cyst had not changed in size or echogenicity. No primary medical condition causing the cyst was discovered. In the end, this use of ultrasound averted a CT and improved patient flow through the ED.

Pearls & Pitfalls for LUQ Ultrasounds
1 Point of Care Ultrasound: The utilization of point-of-care or bedside ultrasound has advanced beyond the simple FAST exam and procedural guidance in the ED. As more providers are becoming comfortable and fascile using bedside ultrasound, we will continue to discover new ways in which it can improve patient care. We are continuing to learn about and research how bedside ultrasound will change the practice of emergency medicine, and what we are doing now is only the tip of the iceberg. This case illustrates one of the sonographic findings you may come across during a bedside abdominal ultrasound. It is important to know what “incidental” findings look like so that the appropriate management options can be considered for your patients.
2 Probe Selection: For most abdominal scanning, you will want to use a low frequency probe (either the phased array or curvilinear transducer). Remember that lower frequency probes provide you with deeper penetration at the expense of resolution.
3 Left Upper Quadrant Window: To evaluate the left upper quadrant, remember to use your acoustic windows. If you are trying to evaluate the splenorenal space, aim your beams through the highly vascular spleen down towards the left kidney. Sweep through the entire left kidney and pan through the entire spleen in this view. If a rib shadow is obstructing your view, turn your probe obliquely so that the indicator is pointing more towards the patient’s back and maneuver your probe in between the rib spaces. You can also have the patient take a deep breath and hold it for a few seconds while you fan your probe anteriorly and posteriorly. Once you’ve visualized the inferior pole of the left kidney and the spleen, slide your probe up a few interspaces in the cranial direction and visualize the left diaphragm and left lower lung fields.
4 Epigastric Window: Place your low frequency curvilinear or phased array probe in a transverse fashion in the epigastric space. Have your patient take in a deep breath to bring the anatomic structures inferiorly below the xiphoid process. The muscular lining of the stomach will appear as a bright white, hyperechoic lining surrounding a dark black, anechoic gastric lumen just to left of midline. A fluid filled stomach can be viewed to assess for gastric distension and to confirm G-tube placement. Often times, the stomach may be difficult to visualize in its entirety because of intraluminal air causing artifacts. The pancreas can also be viewed from the epigastric window but may be obstructed by gas and artifacts arising from the adjacent stomach. Emergency physicians are not currently trained to perform pancreatic ultrasounds in the acute setting, but those who choose to pursue their ARDMS credentialing may find this to be a useful application as resource utilization and emergent imaging is being scrutinized.
5 Practice Makes Perfect: With bedside ultrasound there is no substitute for experience. The more ultrasounds you do, the better you will be able to differentiate abnormal from normal, even when you may not be sure exactly what the abnormality is. An image library of normal and abnormal ultrasounds helps immensely, and we can help. Go to www.EPMonthly.com to find past issues of Soundings and test your ultrasound knowledge.
6 Stay Current: With a tool that is adapting as quickly as ultrasound, it’s essential to keep up to date. You can learn tips and techniques for point-of-care ultrasound through a range of products, from mobile apps to web sites to pocket reference guides.