“Let’s move it, guys, the bus is unloading!” You cringe as you hear the jaded tone in your nurse’s voice. Your department has been especially busy this past month with high-acuity patients, and your hospital is slowly and surely running out of space and resources. Couple all of this with crabby consultants and patients tired of the long wait times, and it is no surprise that your staff and colleagues are getting a little burned out.
Your resident approaches you with the next patient to discuss and you soon find out that the nurses aren’t the only ones who have been bitten by the “burn-out bug”. “This guy is back again…” you can almost feel the exasperation in his voice. “He was just here last week for the same abdominal pain and he’s back again today asking for more pain medications.”
You listen patiently as your resident summarizes his case. The patient is a 45 year-old male who suffered a gunshot wound to his abdomen a few years back. He has had multiple visits to your ED subsequently for chronic abdominal pain and requests for prescriptions for narcotics. He has normal vital signs today and is hunched over and groaning in bed. He moans in pain everywhere you touch him, and he says yes to everything on his review of systems. He continues to beg for IV pain medications and is wondering if he can get IV Phenergan for the nausea and IV Benadryl for the itching he always gets with IV narcotics. The nurses have informed your impressionable young resident that “this is how he always looks” and that “all he needs is some IV Dilaudid and he’ll just get up and walk out soon afterwards”.
You ask your resident, “What’s your plan?” to which he replies, “I just want to get him outta here.” You are surprised by his cynicism so early on in his training. It is only the 2nd month of his second year in EM residency and he’s already feeling jaded. Not good. Not good at all. “Let’s think about what we could be missing here…” you reply. “What’s on your differential for this young man?” Your resident rattles off a list straight out of Tintinalli’s: pancreatitis, appendicitis, diverticulitis, cholecystitis, choledolcholithiasis, nephrolithiasis, AAA, mesenteric ischemia, small bowel obstruction, ileus, diverticulitis, perforated ulcer, gastritis, inferior MI, lower lobe pneumonia, toxin exposure, etc.
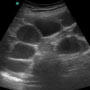
Just for fun, you have your resident wheel in the ultrasound machine into the patient’s room with you as you go in to try to tease out a few more details. As your resident scans through the patient’s right upper quadrant, you discover the patient has no history of gallbladder issues, and the pain is not associated with food or alcohol consumption. Your resident performs a scan of the patient’s kidneys, and you uncover that the patient has no dysuria, hematuria, penile discharge, or flank pain. Moving onto the abdomen, you start questioning the patient about his bowel habits and appetite. Your train of thought is interrupted when you see the ultrasound images your resident gets of the patient’s abdomen (Image 1).
What do you see on ultrasound? Will this patient do well with just IV Dilaudid and an outpatient narcotic prescription this time?
What does the ultrasound show?

Dx: Small Bowel Obstruction
The patient’s bedside ultrasound of his abdomen demonstrates large, dilated loops of small bowel throughout his entire abdomen (Image 2). The loops of bowel are > 3 cm in diameter and are present diffusely in all four quadrants. Right on cue, the patient notes that he hasn’t had a normal bowel movement all week and that he stopped passing gas yesterday. He hasn’t had an appetite over the past few days, and he feels like the sharp, cramping pain he is experiencing, is going to make him vomit.

Your resident changes his tune after seeing the bedside ultrasound images and offers the patient IVF’s, IV pain medications, IV antiemetics, a surgical consultation plus an admission to the hospital for SBO. The surgeons would like a CT scan of the patient’s abdomen before he goes upstairs (of course) and the patient would like an IV cocktail of Dilaudid, Phenergan, and Benadryl (no surprise).
Your shift is coming to an end so you invite your resident out to grab a late night snack to unwind and debrief. Over drinks, you discuss the issues surrounding burn-out in the field of emergency medicine and you offer him some tips on how to keep it at bay:
- Remember and remind yourself why you became a physician.
- Congratulate yourself on the differences you have already made, and the ones you will continue to make in your daily work.
- Make time to take care of yourself and your family.
- Our career as EM physicians should be thought of as a marathon, and not a sprint. Pace yourself and continue to train accordingly.
- Set personal and professional goals and re-evaluate these goals regularly.
Your resident thanks you for the mentoring and the advice, and leaves with a new hop in his step. You take your own advice, order dessert, and reflect about all the good you were able to accomplish in just one ED shift. One day at a time…

Pearls & Pitfalls for performing Ultrasonography to Diagnose Small Bowel Obstruction
01 Save Some Time
Compared to CT or abdominal X-rays, ultrasound can be performed in less than 5 minutes and can significantly increase your pre-test probability for a small bowel obstruction, as well as easily identify ascites in a patient presenting with a distended abdomen. Recent studies suggest that dilated bowel on US had a sensitivity of 91% and specificity of 84% for SBO.
Decreased bowel peristalsis on US was less sensitive (24%) but more specific (98%)1. Use bedside ultrasound to expedite the patient’s emergency department treatment plan. Remember that it is very difficult to determine if the patient has free air on bedside ultrasound. If you are suspicious for perforation, order an upright abdominal or chest x-ray to look for free air under the diaphragm.
02 Getting Started
Use the low frequency (5 to 1 MHz) phased array or curvilinear transducer. You may want to start with a quick FAST scan to ensure there is no free fluid and to identify some intra-abdominal landmarks. Next scan the patient’s abdomen in a systemic manner looking for dilated loops of bowel. It often helps to have the patient point to where it hurts the most and start your scan at that spot.
03 Know What You Are Looking For
In general, large fluid-filled small bowel is relatively easy to see on ultrasound. Experienced ultrasonographers can usually identify these dilated loops based on clinical experience alone. More specifically, previous criteria used for a positive ultrasound includes dilated loops of bowel greater than 25mm in the jejunum or 15mm in the ileum over a length of at least 3 loops. Decreased bowel peristalsis may also be seen, but this can be difficult to identify if you are a novice ultrasonographer.2
04 Avoid Pitfalls
Remember that sensitivity and specificity of ultrasound diagnosis is operator dependent. If your clinical suspicion for SBO remains high after your bedside ultrasound, obtain appropriate imaging and consultation per your department’s protocol. Air-filled loops of bowel can scatter the ultrasound waves and also make it more difficult to identify bowel borders. Remember to use your acoustic windows (spleen, liver, bladder, etc.) and be flexible in how you angle your beam to obtain to the best images possible.
References
1. Jang TB, Schindler D, Kaji AH. Bedside ultrasonography for the detection of small bowel obstruction in the emergency department. Emerg Med J. 2011;28(8):676-8.
2. Unluer EE, Yavasi O, Eroglu O, et al. Ultrasonography for emergency medicine and radiology residents for the diagnosis of small bowel obstruction. Eur J Emerg Med. 2010;17(5):260-4.