Your last patient of the evening is a 42-year-old veterinarian who recently returned from a trip to Mexico where he injured the dorsum of his right hand on a cactus spine. He states that he was able to remove the entire spine and the site subsequently became infected. He put himself on cephalexin and everything improved after a few days. He completed a seven-day course two days ago. Now the infection seems to be returning and he is hoping you could write him a prescription for a stronger antibiotic.
His medical history is pretty unremarkable. His physical exam is only notable for mild rubor, calor, tumor and dolor just proximal to the dorsal right 3rd MCP joint. The puncture site is barely visible. There is no drainage or fluctuance, and you don’t see a pustule. His range of motion is slightly decreased, but all in all, the infection looks pretty mild.
You decide that because things don’t look too bad, he really doesn’t need any IV antibiotics, but you do give him a dose of oral Bactrim along with a Tdap booster that is overdue. Treatment failure leads you to consider a few possibilities. You have some suspicion for a resistant organism, but you’re even more worried that the tip of the cactus spine is still in your patient. An X-ray probably won’t pick it up, CT is probably overkill, as is an MRI, which you couldn’t get after hours anyway. You decide that ultrasound is going to be your imaging modality of choice, as it is especially good at finding wooden foreign bodies.
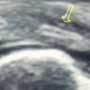
You write your orders, but about fifteen minutes later the nurse comes to you and says that your patient wants to leave now, and it will be at least an hour wait before he can get his ultrasound through radiology. Fearing that either your Press Ganey scores or your malpractice rates could take a hit with your plan-A or your patient’s plan-B, you decide on plan-C. You find the ED ultrasound machine, fire it up, and set the zoom to maximum. You then obtain the following images. The one on top is the infected hand. The other is a comparison view. What do you see? What should you recommend to your patient?
click on image to enlarge
Your ultrasound image demonstrates a magnified view of the head of the metacarpal bone. The cortex is of the rounded head is hyperechoic (bright white), with some posterior shadowing. About 1 millimeter nearfield of the cortex a small, slightly hyperechoic foreign body can be seen (Cactus Spine). There is also a small amount of surrounding tissue edema and a very thin fluid collection, which is less than 1mm thick at its widest point. Comparing to the normal anatomy of the opposite hand is quite useful in this case.
You give the patient the good news that you now know why his infection is back and the bad news that he will need surgery to remove the retained vegetable material. He asks you to call his orthopedist to see if he can go home and have the surgery tomorrow. He gets his wish and leaves happy with the plan.
Pearls & Pitfalls
for Soft Tissue Ultrasonography
1 Probe Choice: Use a high frequency (7.5 to 10 MHz) linear array transducer.
2 Optimize Imaging: Superficial structures are difficult to visualize due to echo reverberations from the transducer. Even with high-frequency transducers, better visualization might be achieved with a standoff pad or liquid interface to provide a better acoustic window. You can try water submersion or a 500ml bag of saline or saline-filled glove sandwiched between two layers of acoustic gel. With water submersion, float the ultrasound probe 1 cm above the skin.
3 Know Normal Structures: It helps to know what normal looks like in order to properly identify abnormal findings. Skeletal muscle will appear hypoechoic with interwoven echogenic striations and hyperechoic fascial planes. Tendons will appear brightly hyperechoic with visible linear fibers on long-axis scanning. Bones will have a very hyperechoic cortex and posterior shadowing.
4 Know Abnormal Structures: Foreign bodies will have different appearance depending on the material. For wood, ultrasound is 90-95% sensitive. A splinter will appear echogenic and produce an acoustic shadow farfield. You can also easily visualize other material such as glass, plastic, and metal on bedside ultrasound. Look for sonographic artifacts such as acoustic shadowing or reverberation artifact coming off the foreign body. If an inflammatory reaction occurs, which usually requires 1-2 days, a black rim of fluid may surround the foreign body and aid visualization.
5 Compare: Use the contralateral side for a comparison view when imaging findings are equivocal
6 Removal Tricks: A short angiocath “finder needle” can be inserted during localization with ultrasound and left in place during to help pinpoint the offending foreign body during removal attempts.
7 Practice Makes Perfect: With bedside ultrasound, there is no substitute for experience. The more scans you do, the better you will be able to differentiate abnormal from normal, even when you may not be sure exactly what the abnormality is. You can find many ultrasound images in the ultrasound section of epmonthly.com
1 EP attendings are able to identify foreign bodies with 98% sensitivity and 70% specificity while trainees had 86 and 83% sensitivity and specificity, respectively. Neither attendings nor trainees were able to accurately identify the number of foreign bodies present in a wou
nd. (Nienaber 2010).
2 Manthey et al., demonstrated far less accuracy with Radiologists evaluating chicken bones, with the sensitivity of ultrasound in detecting gravel: 40%, metal: 45%, glass: 50%, cactus spine: 30%, wood: 50%, and plastic: 40%.
3 Radiography detected foreign bodies generally considered radiopaque (gravel, glass, metal) 98% of the time, but it never detected bodies considered radiolucent (wood, plastic, cactus spine). (Manthey et al.)
4 Turkcer et al., also assessed chicken bones, but found better diagnostic performance with the overall sensitivity, specificity, as well as positive predictive and negative predictive values of plain radiography for both nonradiopaque foreign bodies were 5%, 90%, 33%, and 48%, respectively; those of soft-tissue radiography for both nonradiopaque foreign bodies were 5%, 90%, 33%, and 48%, respectively; and those of ultrasonography for both nonradiopaque foreign bodies were 90%, 80%, 81%, and 89%, respectively.
5 Hill et al., demonstrated intermediate accuracy. Ultrasound detected 44 of 53 foreign bodies (83% sensitivity). Wood foreign bodies were detected 25 of 27 times (93%) and plastic foreign bodies 19 of 26 times (73%). Overall, there were 11 false-positive readings (59% specificity).










1 Comment
i have a thorn stuck in between the ligament between my middle finger and i cant get it out….