It’s busy. There are twenty-eight patients in the waiting room with the longest waiting 4 hours. The queue for CT scans is over 2 hours and the one for ultrasounds is even longer; a staggering 4 hours, plus another hour to get results. Lots of people are frustrated. Your next two patients are both pregnant females in their first trimester with vaginal bleeding. As you perform your H & P, you encounter more similarities between the two. Both have midline crampy pain like a period, with no fever, no vomiting, and no syncope. Both recently had ultrasounds done, one in your ED 3 days ago, and one with her obstetrician four days ago. You know why they are here. One reason – they want to see if their baby still has a heartbeat. You also know that repeating the ultrasound is not really medically indicated using the strict sense of the word. Sure it’s reasonable, even customary, but will it change management tonight? Can’t they just see their OB tomorrow? Is it really the right way to practice medicine to clog up your department even worse while simultaneously adding one more straw to the camel carrying the national healthcare budget? Who are you going to listen to? Press and Ganey? Barack Obama? Your conscience? What will the parents think and how will they react if you tell them, “Sorry, we can’t do an ultrasound tonight. You have to go home and make an appointment tomorrow to see your doctor.”?

Vaginal bleeding in pregnancy, like many things in medicine, is both common and controversial. Do you really need to do a pelvic exam? Do you need to do another ultrasound if they already had one in this pregnancy that showed an IUP and they are not on fertility meds? Few patients will be disappointed if the pelvic exam is skipped, especially if is unlikely to have any important impact on their care, but if you don’t do the ultrasound it may require some explaining if you don’t want them to feel disappointed. But maybe there is a third option. Do a quick bedside ultrasound and show the mom the heartbeat (hopefully). She gets what she wants, you feel like you are doing the right thing, your ED throughput doesn’t take another hit, and you get to improve your ultrasound skills. If sold correctly to the patient and/or her husband, this can truly be a win-win approach.

As long as you know the patient has an IUP, unless they are on fertility meds, for all intents and purposes, you have ruled out an ectopic pregnancy unless the presentation is particularly concerning for a heterotopic pregnancy. It’s even better if someone else has already documented an IUP on a recent scan. Take a look at the two images below. What do they show? Can you quickly and efficiently send the patient on her way home?
What do the images show? Can you quickly and efficiently send the patient on her way home? Conclusion in the following
Dx: Bedside Ultrasound; Mom Leaves Happy
The image on the left shows an IUP at about 10 weeks. The pregnancy was completely within the uterus (not a cornual ectopic, which can mimic an IUP if you don’t scan through the entire uterus and pregnancy sac) and both cardiac motion and gross fetal activity were seen and showed to both parent. This is all that most moms really seem to care about. Show them that their baby looks OK and they will almost certainly leave happy, which was the case with this mom.

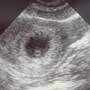
Image 2 shows a very early IUP with a gestational sac and a small forming yolk sac within it. No pole is seen as it is too early. The fluid is anechoic (black) and the sacs are echoic (white). This is also considered definitive of an IUP, but will not necessarily be as reassuring as a heartbeat.

These scans are quick and easy to do in most cases. They are also quite rewarding. Try one on your next pregnant vaginal bleeder before you send her for a formal ultrasound with radiology or gynecology. Then compare what you saw to the formal reading. Once you become confident in your ability to pick out a heartbeat, you may be able to skip the formal ultrasound in certain patients. Happy scanning!

Tips & Tricks for PELVIC ULTRASOUND IN PREGNANCY
01 Probe choice: Use a low frequency linear array transducer (5 MHz) for the transabdominal scan. If you do transvaginal scans, you will need a high frequency intracavitary probe.
02 Know your limitations: Ultrasound may help clarify findings elicited by a thorough history and physical exam. When used correctly, it can lead to a more rapid diagnosis and/or improve diagnostic accuracy, especially for critical conditions or unstable patients. If you are unsure of your findings, get a formal study through radiology or OB/Gyn.
03 Keep it simple: The ED physician rarely needs to do a trans-vaginal scan for evaluation of a pregnancy, especially if the gestational age is greater than 6-8 weeks. With a trans-abdominal you can usually tell if there is an IUP or not (to rule out ectopic), and if there is free fluid or not (to rule out rupture). This, and evaluation for cardiac motion should usually be the extent of a limited bedside ultrasound for the pregnant patient with a pelvic complaint in the emergency department. When you see a definite IUP, your patient would rarely need a formal study done in the ED, especially if they have already had a prior ultrasound documenting an IUP, either in the ED or with their OB. In these cases, save time and money and send mom on her way after you reassure her that everything looks OK. She may need a formal ultrasound at some point in the future however. If you do not see an IUP, see abnormal free fluid, have concerns about the patient’s adnexa, or are unsure about what you saw on your scan, order a formal scan through radiology or OB while the patient is in the ED.
04 Rule out ectopic: An IUP (Intra Uterine Pregnancy) usually rules out an ectopic pregnancy unless the patient is on fertility drugs or your suspicion is very high for a heterotopic. Be sure the pregnancy is in the middle of the uterus. Be cautious of the cornual ectopic, which is the most dangerous type of ectopic. Cornual ectopics develop right at the edge of, but partially within the uterus. Don’t be fooled into thinking it’s an IUP.
05 Know what to look for: A normal uterus is approximately 6 cm long and 3 cm wide. Early in pregnancy the uterus enlarges, but the first clear sonographic sign of pregnancy is usually the gestational sac seen at approximately 5 weeks. Beware of pseudosacs that can be seen with ectopic pregnancies. After the gestational sac forms, the next structure that may be seen is a yolk sac, and soon afterwards you should be able to see a fetal pole. Cardiac activity should be noted within the embryo between 6 to 8 weeks of gestational age during a transabdominal scan. All structures and activity are typically seen 1-2 weeks earlier on transvaginal imaging.
06 Ensure follow-up: Always inform your patient that you are performing a focused and limited beside ultrasound scan to ensure that there is nothing emergent that needs to be cared for immediately and to reassure everyone that the fetus looks ok. Your patient should be advised that a comprehensive follow-up scan should be performed to fully evaluate the pregnancy with their obstetrician as soon as feasible.
07 Experience: With bedside ultrasound, there is no substitute for experience. The more scans you do, the better you will be able to differentiate abnormal from normal, even when you may not be sure exactly what the abnormality is. An image library of normal and abnormal ultrasounds helps immensely, and we can help. Just go to EPMonthly.com and peruse the Ultrasound section for more case studies.
08 Stay Current: Know what the latest recommendations and indications are for performing bedside ultrasounds. The most up to date information and examples on how to document your findings can be found in the new app SonoSupport. Available for iPad and iPhone now.









2 Comments
Where is the disclosure that Teresa S. Wu is the creator and benefits from sales of the SonoSupport app, which is highly touted at the end of this article? This is *highly* unethical.
Otherwise well written.
Dear Raeb,
We apologize that the following disclosures were not included in the online version of the article.
The co-authors of this column are Dr. Brady Pregerson (who manages a free online EM Ultrasound Image Library and is the editor of the Emergency Medicine Pocketbook series at EMresource.org) and Dr. Teresa Wu (who is one of the co-founders of SonoSupport: a mobile app dedicated to improving patient care, education, and enhancing the use of ultrasound worldwide).
We appreciate your feedback and will ensure these disclosures are included in our future articles.
Thanks!