A 54-year-old male is in the ED for a paracentesis because he states he is uninsured and has nowhere else to go. He states his last “tap” was about 4 weeks ago and he is starting to feel short of breath even at rest because of all the fluid. He states these are the same symptoms he always gets and denies any issues that are atypical for him. Just to be sure, you run down a list of pertinent negatives and he politely denies fever, pain, melena, confusion, vomiting, and chest pain. His presentation seems pretty straight forward and you surmise that this is not his first rodeo. Nor is it yours. You let him know that the department is busy so it may take a while to get everything done. You then order some routine labs, the paracentesis set up, and of course, knowing that even a “routine” paracentesis has risks, the informed consent form.
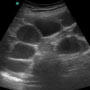
About two hours later you have caught up on your more pressing patient care issues and are ready to do the paracentesis. You look over your patient’s lab work and note the not unexpected low platelet count of 86 and elevated INR of 1.4. “Not too bad” you think to yourself. You confirm that he has signed the consent and walk into the room to get started. Since you recently heard about a patient who bled to death after a paracentesis as a result of a punctured deep abdominal wall varix, you decide to use the technique described by Ault and Rosen to minimize the risk1. This involves looking for abdominal wall varices with the small parts ultrasound probe prior to making the puncture. You start with the curvilinear probe to find a good fluid pocket (image 1) then switch to the small parts probe to look more closely at the abdominal wall where you plan to enter. You obtain the following image with the small parts probe (image 2).


What does image 2 show? Does this appear to be a promising location or should you search elsewhere?
Image 1 was taken with the curvilinear probe and shows ascites, which appears anechoic (black) and is in the near field at the top, as opposed to the intestine, which appears hyperechoic (white) and is in the far field in the mid and lower part of the screen. In real time, you can also often see the bowel moving within the ascitic fluid as it peristalses. Image 2 is only 2.7cm deep and shows a magnified view of the skin and subcutaneous structures. In the labeled version of this image (image 3) there are two round vascular structures, which are both varices (labeled “V”). The varix on the right is close to the surface, and the one on the left is deeper, lying just above the peritoneum. The lower half of the image is black ascitic fluid within the peritoneal cavity. If your needle hits the more superficial varix it might cause a localized hematoma or annoying bleeding from the wound, but not likely anything that would be life threatening. If you hit the deeper varix, however, blood could slowly seep into the peritoneal cavity without any obvious surface bleeding to draw your attention. If this bleeding continued it could become life threatening without any early warning since the bleeding would all be occurring “out of sight”. Image 4 shows the deeper varix in image 3 but was taken after the small parts probe was rotated 90 degrees to get the vessel in the longitudinal orientation. Color-flow Doppler (CFD) was added to further confirm that this is a vascular structure.
Abdominal Wall Varices
Because of these varices, you should definitely search for another site free of these little land mines. Keep in mind that you also want to avoid areas adjacent to any surgical scars, because adhesions in the area may tether down bowel and increase the risk that you will perforate it with your needle. Once you find a safe site, proper positioning for paracentesis is also important. Since bowel floats, it is wise to position the patient with the head of the bed elevated between 45 and 60 degrees. The bowel will rise and the fluid will collect in the lower abdomen. Repositioning the patient after the ultrasound but before the tap, however, is ill advised. Any repositioning may cause the bowel and fluid to move and increases the risk of complications.
You choose a nearby site devoid of abdominal wall varices and perform a 4 liter paracentesis without complication. Your patient is appreciative and thanks you a few hours later when the labs are all back and you finally let him leave. Little does he know that had you chosen your original site to do the puncture he might either be upstairs in the ICU right now or returning soon due to feeling “anemic”.



Pearls & Pitfalls for ULTRASOUND-GUIDED PARACENTESIS
1. Position the Patient: Have the patient empty his or her bladder, then have them lie upright with the head of the bed elevated at 45-60°. This angle allows the bowel to float up and the ascites to collect in the lower abdomen. Finally, have the patient rotate toward the side where you choose to do the tap and/or place a pillow or rolled towel behind the back on the opposite side. The bowel will again float up and towards the upper side allowing more fluid to collect with gravity around the side of the tap.
2. Ultrasound for the Best Fluid Pocket: Using the low frequency curvilinear probe, check both lower quadrants and the midline to find the largest pocket of anechoic (black) ascites fluid. This will often be in the left lower quadrant. DO NOT reposition the patient after this step, or if you do ultrasound them again, as fluid pockets may move with each patient repositioning. Any free flowing fluid within the peritoneal fluid will appear black. Urine, liquid stool, inflammatory fluid and unclotted blood may also appear similar to ascites so correlate clinically.
3. Check for Subcutaneous Varices: You wouldn’t stick a needle into a visible caput medusa would you? Of course not, but occult abdominal wall varices may be present below the surface and the way to visualize them is with the high frequency small parts ultrasound probe. These are especially dangerous when they are close to the peritoneal membrane where they can cause life-threatening but initially silent intra-abdominal bleeding. Varices should appear anechoic and be compressible. Use of color-flow Doppler can also aid in visualizing and avoiding subcutaneous varices. If they are present under your initial tap site of choice, abandon that location and use the small parts probe to scan for a safer area.
4. Do the Tap: Most practitioners will localize a fluid pocket with ultrasound and then finish the procedure “blind”. Alternatively you may use a sterile probe cover to visualize your procedure in real time. If you chose the latter, you may want to have an assistant hold the ultrasound probe for you so that you have use of both of your hands. If fluid stops flowing but you think or see that there is a lot more, one or more of the following techniques may help you get more of it out: reposition the patient so fluid settles with gravity around the needle; flush the pigtail catheter to push away bowel that may have been sucked onto the fenestrations; partially remove the catheter.
References
Ault, Mark J, Rosen, Bradley T, “Out of Sight Should Not Be Out of Mind: What Lurks Just Beneath the Surface of the Cirrhotic Abdominal Wall”, ICU Director 2012:3 p.128-129
Images courtesy of Mark Ault, MD, Cedars-Sinai Medical Center