“Are you sure I don’t need that magic stroke medication that I saw on TV?” you hear a patient ask through the curtains in your acute care area. “I am within the 3-hour window.” You pause to listen to your senior resident reassure the patient that she is not having a stroke and explain to her the risks and benefits of that “magic stroke medication”. Within a few steps, one of your nurses stops you to tell you that your patient in room 19 wants to talk to you about a prescription for Plavix because he read an advertisement in the newspaper telling him that it can prevent him from having a heart attack. “Isn’t room 19 here for a sprained ankle?” you ask. Your nurse simply throws her hands up and shrugs as she gives you the “It’s your problem” look.
You begin to wonder how the practice of medicine is going to change now that all of your patients have become mainstream media mavens. As if he read your mind, one of your chief residents approaches you with another patient request prompted by something he saw on television. You walk into the patient’s room with your chief resident, politely introduce yourself, and ask how you can be of service. The patient explains that he was playing in a pick-up game of basketball today when he was suddenly shoved from behind. He fell forward and landed on his right knee. He hasn’t been able to bear weight on the knee, and he’s concerned about the intense pain and swelling. On exam, you suspect he has an effusion and you note he is unable flex the joint to 90°.
Your patient meets multiple criteria of the Ottowa knee rule, so it’s a no-brainer that he is going to require imaging of his injured knee. As you are explaining to him that you are going to order an X-ray, the patient interjects with “Can’t you do an MRI or an ultrasound of my knee instead? I read someplace that too much radiation can cause cancer and I saw the doctors on Grey’s Anatomy do an ultrasound on someone’s leg once.” You stifle a smile, and tell the patient, “That’s an excellent idea,” as your resident walks out of the room to grab the ultrasound machine.
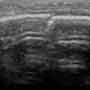
With your patient lying supine on the gurney, you perform a bedside scan of the patient’s unaffected left knee first so that you can show him and your resident what a normal baseline is. You then proceed to capture the following images of his injured right knee.


What do you see on his bedside knee ultrasound?
Conclusion in the following
Dx: Fracture Visible on Musculoskeletal Ultrasound


You listen proudly as your resident explains to the patient that there is a break in the cortex of the patella on your bedside scan (bottom). The resident then points out the heterogeneous peripatellar fluid collection that is likely a hemarthrosis that developed following his patellar fracture (top). You begin cleaning off the linear array transducer as your resident explains to the patient that he would still recommend an X-ray to evaluate the extent of the fracture and to assess for other associated injuries. The patient seems impressed with your team’s clinical acumen and resource utilization and agrees to have the X-ray taken. You are thrilled that you were able to satisfy the patient’s non-traditional expectations with bedside ultrasound, and excited that your resident has become so proficient with his scanning skills. But nothing made you happier than hearing your patient state on the way out, “Wow, you guys are even smarter than that doctor on House! I can’t wait to tweet to my buddies about how cool ultrasound is!”
Pearls & pitfalls for Musculoskeletal Ultrasound
1. DO YOUR HOMEWORK: More and more practitioners are using bedside ultrasound to obtain valuable data that can be used to enhance and expedite patient care. It is important to recognize the limitations of bedside ultrasonography and to stay current with the recent literature. Update your skills regularly and continue to challenge yourself by reading, scanning, and attending advanced courses.
2. AUGMENT CARE: Although ultrasound is not the first-line imaging modality used to detect acute bone fractures, in situations where X-ray is not readily available, bedside ultrasound can be used to provide useful information that can help augment patient care.
3. HIGH FREQUENCY: Most musculoskeletal applications are best performed using a high frequency linear array transducer (13-5 MHz). Remember that high frequency probes allow better visualization of superficial structures.
4. CREATING THE IDEAL SURFACE: Apply a copious amount of gel over the target surface to be scanned. To improve your acoustic window over superficial structures, use water immersion or create an acoustic standoff pad (this can be done with a 500ml bag of saline with gel on both interfaces or a water-filled glove sandwiched between two layers of gel).
5. ASSOCIATED UNDERLYING FRACTURES: An acute hemarthrosis will appear anechoic (black). As clot begins to form within the effusion, it will become more hyperechoic and heterogeneous in appearance. Whenever a traumatic effusion is visualized, always search for an associated underlying fracture.
6. BONES: Bones will appear bright white (hyperechoic) on ultrasound. An acoustic shadow will be noted farfield to the bony cortex.
7. ASSESSING FOR ACUTE FRACTURE: To assess for an acute fracture, scan along the hyperechoic cortical line in search of any break in the cortex. If a cortical irregularity is noted, correlate your sonographic findings with the physical exam. Note that large nutrient vessels can also appear as hypoechoic cortical irregularities on ultrasound. Pressure with the probe or palpation over the noted irregularity should cause pain if the irregularity noted is secondary to an acute fracture.
8. EVALUATING THE CORTEX: To fully evaluate the cortex, scan along the target bone systematically in multiple planes. If you are unsure of findings, use the opposite side for a comparison view.
9. BEDSIDE ULTRASOUND AND PEDIATRICS: Ultrasound diagnosis of fractures has been studied in all long bones and also many of the wrist bones, ankle bones, ribs, and cranium. Over the past few years, ultrasound has gained increased popularity in its ability to diagnose acute fractures in the immature skeleton of children. Because many pediatric fractures are managed non-operatively, many practitioners are using bedside ultrasound to not only make the diagnosis, but also to aid with reduction and splinting.
10. PRACTICE: Remember that practice makes perfect. With bedside u
ltrasound there is no substitute for experience. The more ultrasounds you do, the better you will be able to differentiate abnormal from normal, even when you may not be sure exactly what the abnormality is.