Emergency physicians stand as the front line in recognizing dangerous emerging polydrug trends, such as desomorphine
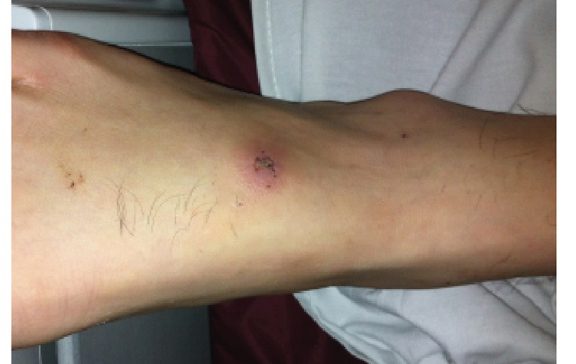
Case: A 41-year-old male with rheumatoid arthritis, depression and polysubstance abuse is brought to an urban emergency department after being found unresponsive at home. In the field, paramedics administered 2mg of nebulized naloxone and the patient became more alert. Per the patient’s spouse, they had been injecting “crocodile” all week. Patient also admitted to taking Xanax and methadone. While in the ED, he required two doses of naloxone 0.8mg nebulized and an additional dose of 0.4mg IV over the course of 1.5hrs. Laboratory data were within normal ranges aside from a urine drug screen positive for both benzodiazepines and methadone but negative for opiates. Vital signs: BP 155/89, HR 69 and RR 10. Physical exam was significant for somnolence, pinpoint pupils and small (<1 cm) healing ulcers on the bilateral lower extremities where the patient had injected (see photos). Patient was started on a naloxone drip at 3 mcg/kg/hr (0.21mg/hr) and admitted to the ICU.
“Krokodil” – which is the Russian word for Crocodile – is a home-made injectable opioid that originated in Mother Russia in the early 2000’s1. Krokodil’s main psychoactive substance is desomorphine. Desomorphine was first synthesized in 1932 and is 8 to 10 times more potent than morphine. It has faster onset of action and a shorter duration of action than morphine2. During the production of Krokodil, desomorphine is synthesized from codeine-containing-tablets using a process that involves solvents such as gasoline or lighter fluid, iodine, hydrochloric acid, and red phosphorus obtained from matches3.
This concoction typically goes unpurified and unfiltered – it is simply drawn up into a syringe and injected – which means that the potential for skin and soft tissue damage is substantial. Effects such as gangrene, thrombophlebitis, ulcerations, and infections resulting from injection of this homemade opioid has given users dermatologic findings similar in appearance to a crocodile’s scales (hence the name). Since Krokodil is made from codeine tablets that contain additional substances such as dyes, coatings and other drugs, patients are potentially injecting these in addition to the components of the chemical synthesis. The injection of these extremely polluted solutions has resulted in reports of systemic complications, neurological symptoms such as impairments in motor skills and memory, and early death3.
Case Resolution: After discussion with the patient, he related that he had bought heroin. He had purchased it as a powder, cooked it up, and injected it. He then developed some small sores around his injection sites and therefore inferred that it was Krokodil, based on a news report he’d seen on television.
Case Discussion: This patient’s presentation was more consistent with a longer acting CNS depressant, reversible by naloxone, such as methadone. He required multiple doses of naloxone and ultimately an intravenous drip. Like fentanyl, desomorphine has a very fast onset of action and a half-life of about two hours, thus it is unlikely that his prolonged respiratory depression was due to desomophine4. There seems to be a fear in the drug community that any tissue and or skin damage at injection sites could mean contamination of their drug with Krokodil.

In countries such as New Zealand, where heroin is expensive and supply is unreliable, homemade opioid injectables predominate the injection drug scene5. Likewise, a combination of social and governmental factors in Russia has resulted in the rampant spread of Krokodil use. Poor support for injection drug users, substandard medical treatment, and a government that forbids opioid substitution therapy likely all contribute to this drug burden in Russia and other post-Soviet countries3. Until July 1, 2012, over-the-counter tablets containing codeine were available in Russia1. This has led to a decrease in Krokodil use since November 2012. In the Ukraine, Krokodil use has decreased from 60 to 40% of polydrug injectors and 20 to 5% in users of Krokodil only6. In the US there have been isolated reports of individuals obtaining home bake methods for Krokodil on the internet7. Ultimately, it is unlikely that Krokodil will reach the epidemic proportions in the United States that it has in Russia given that codeine is not readily available on the street and heroin remains relatively cheap. However, it is important for EM physicians to be aware of international drug abuse trends since EDs are the front-line for monitoring sentinel cases nationally.
References
1. Gahr M, Freudenmann RW, Hiemke C, Gunst IM, Connemann BJ, Schönfeldt-Lecuona C. “Krokodil”—Revival of an old drug with new problems. Subst Use Misuse. 2012;47:861-3.
2. Eddy NB, Halbach H, Braenden OJ. Synthetic substances with morphine-like effect: Clinical experience; potency, side-effects, addiction liability. Bull World Health Organ. 1957;17(4-5):569-863.
3. Grund JP, Latypov A, Harris M. Breaking worse: The emergence of krokodil and excessive injuries among people who inject drugs in eurasia. Int J Drug Policy. 2013;24(4):265-74.
4. Skowronek R, Celiński R, Chowaniec C. “Crocodile” – new dangerous designer drug of abuse from the east. Clin Toxicol. 2012;50:269-.
5. Harris M. The ‘do-it-yourself’ new zealand injecting scene: Implications for harm reduction. Int J Drug Policy. 2013;24(4):281-3.
6. Booth RE. ‘Krokodil’ and other home-produced drugs for injection: A perspective from Ukraine. Int J Drug Policy. 2013;24(4):277-8.
7. Castillo M. Ariz. poison control center reports first U.S. cases of krokodil use. 2013
8. Drug Enforcement Administration Office of Diversion Control Drug & Chemical Evaluation Section. Desomorphine. 2013;2013