It is the processing of the sickest patients, the ones who are admitted to the hospital or transferred for admission at another hospital, that determine the overall flow rate of the emergency department. As a result, less sick patients – those who can be treated and released – benefit from the rapid flow processing of the sicker set.
It is the processing of the sickest patients, the ones who are admitted to the hospital or transferred for admission at another hospital, that determine the overall flow rate of the emergency department. As a result, less sick patients – those who can be treated and released – benefit from the rapid flow processing of the sicker set.
It is the processing of the sickest patients, the ones who are admitted to the hospital or transferred for admission at another hospital, that determine the overall flow rate of the emergency department. As a result, less sick patients – those who can be treated and released – benefit from the rapid flow processing of the sicker set.
The United States Government Accounting Office found this same concept applicable to emergency departments in the report to Congress in 2009 [1]. The ED and its physicians are increasingly responsible for patient flow into (and through) the hospital. As previously reported, 68% of inpatients are processed through the ED, so this important front door to the hospital must be operating efficiently for the hospital to accomplish its mission. For this reason, it is critical that emergency physicians develop flow processes for seriously ill and injured patients.
The Emergency Department Benchmarking Alliance (EDBA) developed and published the definitions that are being used to measure the performance of EDs in regard to admitted patients [2]. The Centers for Medicare and Medicaid Service (CMS) has further refined these definitions that relate to the care of patients who are admitted to the hospital, and hospitals now publish these measures and the results are subject to media attention [3]. The Joint Commission has also promoted the importance of ED flow, and minimizing ED boarding.
Admitted patients and flow, by the numbers

The EDBA data survey was compiled with the data from 1,026 EDs that saw 40 million patients in 2012. The performance measures related to admitted patients are presented in Table 1. As with other results from the survey, there are significant differences in performance that are volume related. EDs with adult populations are higher acuity, with higher admission rates. High volume EDs admit more patients and transfer a lower percentage. Their processing times are longer for admitted patients, including almost double the length of boarding those patients.
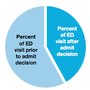
Emergency physicians and ED leaders are able to easily define and characterize the first column of numbers. This is the percentage of all ED patients seen who are either moved to an inpatient area for full admission, or for observation. The second column is the percentage who are transferred (following EMTALA guidelines) to another medical facility.
The median length of stay for admitted patients includes all aspects of moving those patients through the ED. Flow includes the total time from patient arrival and recognition as a patient, through the time to con- tact with a mid-level or physician provider, to the time of decision regarding disposition, to the time of patient movement out the doors of the ED to the inpatient unit. It is best expressed as a MEDIAN time, as with all time elements in the ED process. Hospital and ED leaders will recognize this as CMS Clinical Quality Measure ED-1 (and NQF 0495).
Included within this measure is the time measure ED-2 (NQF 0497), or in CMS language: Median time (in minutes) from admit decision time to time of departure from the ED for patients admitted to inpatient status. This is the length of boarding of an inpatient in the ED. This time interval has been difficult to implement because of the variability in the definition of the first time marker. There is little agreement between hospitals about the definition of “admit decision time”. It is even more difficult when the ED leaders try to collaborate with the overseers of the hospital’s computer system to identify this marker. Despite the difficulties, the relationship of boarding to the volume of patients seen in the ED, and its relationship to overall patient flow, are very important.
The leaders at CMS are aware that there are significant differences in ED boarding based on volume, and are looking for ways to improve the Hospital Compare website and other reports, to account for cohorts by volume and acuity. From the data they have studied, it is recognizable that there are significant differences in the ability of very large, high acuity EDs and very small EDs to move admitted patients to inpatient units.

It is critical for ED leaders to improve flow of admitted and transfer patients. There are now numerous publications that offer suggestions to improve flow of the sickest patients. A couple of examples:
1. Reduce blocking behaviors by staff in admitting units. This includes processes where ED nurses give report by electronic means (fax or computer) and the patient is transported to the inpatient unit. No need to have a unit “accept” a patient.
2. Conform to pre-planned EMTALA guidelines for transfer patients, using a prepared package of documents. This insures that all elements of the transfer process are completed, and allows the nurse and unit clerk to expedite the transfer process, reducing bed time for these patients.
3. Develop improved working relationships with hospitalists. This includes incorporating hospitalist leaders in emergency department meetings, developing structured admission communications, and using daily “bed huddles” with the hospitalists to plan for admissions.
Communities that utilize EDs heavily for the management of persons with mental health and substance use problems are investigating processes and sites of care other than the hospital. Some communities have alternate sites of care for patients with primary mental health issues other than the ED. A recent development is the adoption of “sobering centers” that are used as sites of observation and care for those individuals with a problem that is primarily related to intoxication. These sites may be funded and staffed by law enforcement, EMS, faith-based organizations, and community volunteers [4]. That relieves the ED of those patients occupying beds, and the time of ED nurses and techs.
The timely processing of the patients who are admitted to the hospital or transferred for admission to another hospital, improves the overall flow rate of an emergency department. This is the leadership opportunity for emergency physicians, and one that allows for improved service to all patients who arrive for ED service.
REFERENCES
1. Hospital Emergency Departments: Crowding Continues to Occur, and Some Patients Wait Longer then Recommended Time Frames. United States Government Accounting Office. GAO-09-347. April 2009
2. Emergency Department Performance Measures and Benchmarking Summit. Welch S, Augustine J, Camargo CA, et al. Acad Emerg Med (United States), 2006 Oct;13(10):1074-80
3. Hospitals With the Shortest ED Wait Times. Rizzo, Ellie. Becker’s Hospital Review. October 29, 2013
4.First New Year’s Eve could be interesting for Houston’s new sobering center. Hlavaty, Craig. Houston Chronicle. December 31, 2013
Dr. Augustine is the Vice President of the ED Benchmarking Alliance.