This landmark trial suggests that complex, invasive sepsis care brings no statistical mortality benefit while consuming healthcare resources. Here is a quick run-down of the study that is shifting the sepsis conversation.
This landmark trial suggests that complex, invasive sepsis care brings no statistical mortality benefit while consuming healthcare resources. Here is a quick run-down of the study that is shifting the sepsis conversation.
The ProCESS Trial in Brief
This landmark trial suggests that complex, invasive sepsis care brings no statistical mortality benefit while consuming healthcare resources. Here is a quick run-down of the study that is shifting the sepsis conversation.
It’s been over 12 years since the landmark publication by Dr. Manny Rivers describing a protocol-based algorithm for treatment of patients with septic shock. Despite the age of this study it has remained a staple for emergency medicine residency journal club review. Among other things, the Rivers study highlighted the need to identify septic shock early, and this had significant downstream effects. It brought ICU-level care to the ED and forever changed the way we managed sick patients from the moment they hit the door.
 As with many things in medicine, these sepsis guidelines have been plagued with controversy. Multiple studies have called into question whether such aggressive transfusion rates were necessary given their inherent risks. While many large academic centers have all the fancy high-end gadgets to go with the protocol, does that mean that those of us practicing at smaller, community-based hospitals are providing substandard care?
As with many things in medicine, these sepsis guidelines have been plagued with controversy. Multiple studies have called into question whether such aggressive transfusion rates were necessary given their inherent risks. While many large academic centers have all the fancy high-end gadgets to go with the protocol, does that mean that those of us practicing at smaller, community-based hospitals are providing substandard care?
It is with this controversy front and center that emergency physicians anxiously awaited the results of the ProCESS trial, which was published in March. Would it fundamentally change the way we treat sepsis? Here is a cheat sheet of what they did, and what they found.
ProCESS was a multicenter, randomized trial, conducted at 31 academic centers all with an annual census of at least 40,000. All centers had to have the ability to perform screening lactates to identify patients with cryptogenic sepsis. To be eligible they had to be over 18 and meet their criteria for septic shock. 1351 patients underwent randomization into one of three groups: EGDT, their standard protocol, or the usual care. Randomization occurred with virtually identical baseline demographics across all three groups. The EGDT group protocol mimicked that of Dr. Rivers protocol. The standard protocol group required only 2 large-bore IVs (central line if unable to get reliable IV access), fluids, antimicrobials, and pressors if fluids failed to reach BP targets. The usual care arm essentially allowed the bedside provider free-reign to direct all resuscitation efforts without any protocol guidance.
Their primary outcome was all-cause mortality at 60 days. There were no statistically significant differences in mortality rates across all three groups: EGDT (21.0%), protocol-based (18.2%) and usual care (18.9%). How about at 90 days? No difference. How about discharge location? No difference. It is worth noting, though, the EGDT group had higher rates of ICU admission and higher rates of blood transfusion. So while there was no mortality difference, the EGDT group did consume more resources.
In the Rivers et al. study their 60-day mortality in the standard therapy was 57% in the usual care group and 44% in the EGDT group. So why the huge difference compared to the ProCESS groups? Most likely it’s because one thing we learned from the Rivers study: the need for rapid, early identification. Lactate studies are now almost ubiquitous. In the ProCESS group, 96% received fluids early, and an astonishing 97% received antibiotics in the first 6 hours.
So what does this mean going forward? It means that the things we postulated for many years have panned out – it’s really all about early identification, early fluids, and early antimicrobials when it comes to saving lives. While prior data suggested this, it’s time for everyone to get on board. You don’t need a complex algorithm, invasive and painful procedures, or expensive equipment to provide good care. And now you have the data to prove it.
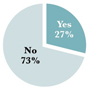
Q. How is sepsis currently handled in your emergency department?
1 Australia
We use rapid assessment; bloods including 2 sets of cultures; early fluids, antibiotics, etc… then ionotrope therapy if needed after ~ 2 litres of IVF.
Andrew Watson
2 Bahrain
We follow early goal-directed therapy (EGDT). The ProCESS trial will NOT change this sepsis management.
Ankur Verma
3 Belgium
We use rapid infection source identification (cultures/lab/radiology); oxygen en rapid fluid administration; rapid antibiotics; rapid ICU transfer (if possible, often not); arterial line; ET/niBPAP if needed; SwGz never placed on ED; CV catheter quit often placed for inotropics (no CO measurement, no central venous oxygen follow up, blood gases (with lactate) followed frequently.
Turn over +/- 2 hours for above, transfer to ICU 2-6 hours.
Ankur Verma
4 Brazil
ProCESS will not change our sepsis management. We give antibiotics in the first hour; Volemic reposition with goal of MAP > 65 mmHg in the first hour;
vasopressor if necessary.
Rodrigo Antonio Brandão Neto
5 Dominican Republic
The ProCESS trial will change how we handle sepsis. Currently we use early identification via sirs/sepsis criteria, severity determination with vitals/end organ/lactic acid; Aggressive fluids resuscitation; Early antibiotics; EGDT;
Effectiveness reassessment via lactate clearance, and end organ function.
Amado Alejandro Baez, MD
6 France
We obey the sepsis guidelines from 2013. ProCESS won’t change this.
AK
7 Germany
We have a sepsis guideline – early recognition and resuscitation are key (“early goal directed therapy”). As soon as sepsis is considered, antibiotic therapy is started.
Andreas Huefner
8 India
The ProCESS trial will change our sepsis management. We followed early goal-directed therapy (EGDT).
Dr. Asit Misra
9 New Zealand
Screening tool for sirs in use with uptriage for those with 2 criteria, cultures, lactate, abx, and 1rst liter of fluid. Patients are to be seen in 10 minutes. Renee Garcia
10 Qatar
We more or less follow practice consistent with the third arm (i.e. the non-protocol) arm of PROCESS trial, so it will NOT change how we handle sepsis.
Dharmesh Shukla
Our sepsis management varies. It does not involve scvo2 catheter or dobutamine. Early antis plus fluid plus source control emphasised. Inotropes and antibiotics very variable. Fluid management variable…. Process trial will make people focus on the basics of good supportive care.
Peter Cameron, MD
11 Saudi Arabia
ProCESS will change our management. We give Abc, fluid, Abx, ICU. Some attendings still give EGDT
12 South Africa
We use early antibiotic treatment (preferably within one hour); Judicious fluid management; Test to evaluate source started in the ED; Admission as soon as possible for further treatment in the hospital. ProCESS will NOT change how we operate.
Anita Groenewald
13 South Korea
Our department cares for sepsis patients in collaboration with several other departments in the hospital. ED triage, check all labs, blood cultures and all films including CT or MRI without delay. Give broad spectrum antibiotics, shock management, etc… If surgery required, directly call the surgery department and admit to ICU.
Sam Beom Lee, MD
14 Sudan
We manage sepsis according to the surviving sepsis campaign guidelines of 2012. ProCESS will not change what we do.
Abderrhman Alnour Alimam
15 Sweden
We use standardized protocols (in conduct with EGDT) for sepsis and septic shock. The protocols are very sensitive for sepsis and are also helpful to detect those patients that are at risk for deterioration, and maybe we overtreat some patients. The protocols stress immediate fluid resuscitation. Since we are obliged to see all patients within an hour of arrival to the ED, the chance of early detection of sepsis is quite high. Unfortunately we have not studied if the protocols we use (since 2012, developed locally by an emergency physician) have changed the outcome for septic patients at our hospital. Sepsis is of course common, but the patients presenting with septic shock are quite rare in our ED.
Frida Meyer
16 Turkey
The ProCESS trial will NOT change our sepsis management. We currently handle sepsis like the second group in the ProCESS trial. Intensive therapy, but only rarely using a central line.
John Fowler, MD
17 United Arab Emirates
The ProCESS trial WILL change our sepsis management. Currently we use EGDT Protocol following the Surviving Sepsis Guidelines – strictly adhered to with compliance measured as a Key Performance Indicator (KPI).
Bob Corder, MD
18 United Kingdom
The ProCESS trial won’t change our sepsis management. We currently handle sepsis with EGDT.
Luca Pensabene
19 USA
Fluid resuscitation–strict I&O; Moisturized O2; Vasopressors if needed; Antimicrobials quickly-following; cultures–also done quickly; Steroids if indicated; Non-invasive respiratory support unless too ill–then RSI and vent. Unless DNR or DNI. Warming patient (BAIR hugger) if needed (or if not available-warm blankets loosely over patient with another over blanket to form “pocket of air”). Anxiolytics if needed; Pain control if needed.
Heidi Steventon Rothenberg, MD
EPI Journal
Read more stories of global emergency care development at www.epijournal.com