With the baseball and softball seasons well underway, you are likely to encounter children with arm pain in the emergency department. Injuries to the elbow and shoulder in the pediatric throwing athlete are relatively prevalent and result from a variety of factors, including skeletal immaturity, poor mechanics, and overuse.
With the baseball and softball seasons well underway, you are likely to encounter children with arm pain in the emergency department. Injuries to the elbow and shoulder in the pediatric throwing athlete are relatively prevalent and result from a variety of factors, including skeletal immaturity, poor mechanics, and overuse.

Between Little League and summer camps, emergency physicians need to know how to appropriately treat arm injuries in young throwers.
With the baseball and softball seasons well underway, you are likely to encounter children with arm pain in the emergency department. Injuries to the elbow and shoulder in the pediatric throwing athlete are relatively prevalent and result from a variety of factors, including skeletal immaturity, poor mechanics, and overuse. Here we will present a few of the common upper extremity conditions that you may see, in addition to a brief discussion on prevention and treatment.
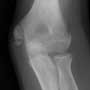
Case 1: A 12-year-old baseball pitcher presents with 4-6 weeks of gradually worsening right elbow pain that became acutely worse after his last pitch. He thinks he felt a “pop.” There is non-radiating pain and tenderness over the medial aspect of the elbow, directly overlying the medial epicondyle. The pain is made worse during your exam with wrist extension and valgus stress of the elbow. He has limited range of motion and is unable to fully extend the elbow. His radiograph is shown.
Mechanism of injury: Overuse injuries result from excessive or maladaptive stress that can be due to poor mechanics and
inadequate rest. These repetitive stresses are further exaggerated by weak links in the kinetic chain as well as the open growth plate. Medial-sided elbow injuries are most common due to the valgus stress and distraction force created by throwing. Furthermore, the medial epicondyle growth plate region begins to ossify at about five years of age, but may not close fully until almost 16 years of age. Injuries to the medial elbow in children include apophysitis (aka Little League elbow) and avulsion fractures. In contrast, skeletally mature athletes often sustain muscular or ligamentous (i.e., ulnar collateral ligament) injuries as a result of these same forces across the joint.
Contralateral compression of the radiocapitellar joint with elbow extension can cause lateral-sided elbow pathology, such as osteochondritis dessicans and avascular necrosis (Panner disease). In one prospective study of youth pitchers, roughly 5% of children ages 9 to 14 sustained a serious elbow or shoulder injury that required them to have surgery or to quit playing.
Little League elbow: If radiographs are normal or show only mild physeal widening or an irregular ossification, then apophysitis is the likely diagnosis. This is treated with RICE (rest, ice, compression, elevation), oral anti-inflammatory medications, and cessation of throwing for at least 4-6 weeks. Once the pain resolves, the athlete may gradually return to play under close supervision with rehabilitation. A change in position may be considered, and pitch counts should be monitored closely.
 Medial Epicondyle Avulsion Fractures: The radiograph to the left demonstrates an avulsion fracture of the medial epicondyle. If the medial epicondyle is avulsed and displaced 3mm, ulnar nerve symptoms, or loose bony bodies in the joint, then surgery is often considered. However, the degree of displacement requiring operative intervention remains controversial. Nonoperative management of the case described resulted in a good outcome. In adults with ligamentous injuries, conservative treatment with rehabilitation is recommended except in high-level or high-demand throwing athletes. The reconstructive surgery performed is the well publicized “Tommy John” surgery.
Medial Epicondyle Avulsion Fractures: The radiograph to the left demonstrates an avulsion fracture of the medial epicondyle. If the medial epicondyle is avulsed and displaced 3mm, ulnar nerve symptoms, or loose bony bodies in the joint, then surgery is often considered. However, the degree of displacement requiring operative intervention remains controversial. Nonoperative management of the case described resulted in a good outcome. In adults with ligamentous injuries, conservative treatment with rehabilitation is recommended except in high-level or high-demand throwing athletes. The reconstructive surgery performed is the well publicized “Tommy John” surgery.
Case 2: A 14-year-old catcher presents with several weeks of progressive right shoulder pain with throwing. Examination reveals full active range of motion, full strength of the rotator cuff, and tenderness at the proximal humerus. Shoulder radiographs demonstrate very slight widening of the proximal humeral epiphysis.
Little League shoulder: Similar to the elbow, shoulder pain is a common complaint among young throwers. The proximal humeral epiphysis does not close until the late teenage years and is often subject to repetitive stresses with maximal external rotation during the throwing motion. Progressively worsening upper arm pain with throwing is frequently attributed to proximal humeral epiphysiolysis, or Little League shoulder. Physical exam will usually reveal tenderness at the proximal humeral physis, while weakness and significant loss of motion are unlikely. Radiographs may demonstrate widening of the physis, or sclerosis, fragmentation, or cystic changes of the proximal humeral metaphysis. Although overuse and inadequate rest are major culprits, pre-existing deficits in glenohumeral internal rotation and scapular dyskinesis contribute to this problem. Therefore, treatment is
focused on both relative rest from throwing and active rehabilitation.
Glenohumeral instability presents another problem in the young throwing athlete and may be traumatic or atraumatic in origin. Ligamentous laxity allows for excessive translation of the humeral head, resulting in repetitive microtrauma and pain. In atraumatic cases, a program of rehabilitation is recommended, while surgical stabilization may be required for traumatic instability (i.e., glenohumeral dislocation), especially for recurrent episodes. Although injuries to the rotator cuff and the glenoid labrum may occur, they are much less common in adolescent athletes compared to adults.
Treatment and Prevention: In the absence of significant radiographic findings, the treatment of shoulder or elbow pain in the young athlete invariably includes rest from throwing. Because overhead athletic activities require coordinated movements of a complex kinetic chain, rest is often accompanied by a structured rehabilitation program to address deficits in glenohumeral motion, scapular function, and core strength. Once symptoms are resolved, return to throwing commences in a gradual, supervised fashion. It is well understood that the quantity of throwing correlates directly with injury, so particular attention should be paid to providing adequate rest during the season and adhering to pitch count regulations.
Healthcare providers, including emergency physicians, must be vigilant about recognizing the warning signs of overuse injuries in the pediatric population. Early detection of these upper extremity conditions and appropriate counseling is important in minimizing further harm to the young athlete. Rather than simply allowing these patients to return to sports after a brief period of rest, consider referring them to a sports medicine specialist for more comprehensive evaluation and management. For more information on injury prevention in youth sports, visit the STOP Sports Injuries Campaign website at
www.stopsportsinjuries.org.
Jeffrey Feden, MD & Jonathan H. Valente, MD work in the Division of Sports Medicine at The Alpert Medical School of Brown University.
References
- Chorley J (2012, September 6). Elbow injuries in the young athlete. Retrieved April 1, 2013 from UpToDate online textbook: http://www.uptodate.com.
- Greiwe RW, Saifi C, Ahmad CS. Pediatric sports elbow injuries. Clin Sports Med 2010;29:677-703.
- Fleisig GS, Andrews JR, Cutter GR, et al. Risk of serious injury for young baseball pitchers: A 10-year prospective study. Am J Sports Med 2011;39:253-7.
- Mariscalco MW, Saluan P. Upper extremity injuries in the adolescent athlete. Sports Med Arthrosc Rev 2011;19:17-26.