 Are Tasers a safe alternative to lethal force, or are they dangerous weapons associated with dysrhythmia and sudden cardiac death? Everything you need to know to treat the taser victim in the ED.
Are Tasers a safe alternative to lethal force, or are they dangerous weapons associated with dysrhythmia and sudden cardiac death? Everything you need to know to treat the taser victim in the ED.
Are Tasers a safe alternative to lethal force, or are they dangerous weapons associated with dysrhythmia and sudden cardiac death? Everything you need to know to treat the taser victim in the ED.
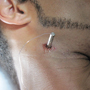
A 52-year-old male was transported to the emergency department by ambulance after resisting arrest. He was subdued by police with a Taser, and arrived complaining of a Taser dart in his neck (photo), as well as his right anterior chest. He denied any other trauma, including closed head injury or loss of consciousness. He also denied difficulty breathing, swallowing, or speaking. On physical exam, the patient had normal vital signs and no respiratory distress. There was no active bleeding around the Taser darts. He had normal lung sounds, and no hematoma was appreciated in association with his wounds.

Background
In 1974 Jack Cover developed the Thomas A. Swift Electrical Rifle (TASER), named after his childhood hero, Tom Swift, the central character in a series of adventure novels. The Taser is now the most common conducted electrical weapon used by law enforcement agencies to quickly incapacitate violent or combative individuals. It uses compressed nitrogen to fire two dart-like electrodes that remain attached to the device by conductive wires. The sharp portion of the Taser dart is approximately 9mm in length. It delivers a 5 second burst of stimulation, with an initial arcing voltage of 50,000 V. The peak voltage experienced by the subject is 1,200 V, at an average current of 2.1 mA1. The shock is delivered in 100 ms pulses, functionally inhibiting alpha motor neurons, preventing voluntary movement and contributing to uncontrollable skeletal muscle contraction for the duration of the discharge.
The exact pathophysiology of electrical injury is not fully understood. While higher voltage does correlate with increasingly severe electrical burns, it is the strength of the current (amperage) as well as the circuit resistance that typically determine the morbidity and mortality associated with these injuries. Even exposure to the relatively low 110 V current found in most households (e.g. from a blow-dryer) has caused fatalities under circumstances of low resistance and high current (such as bathtub related injuries). In the United States the standard alternating current (AC) frequency is 60 Hz. At this frequency, the threshold for perception of a shock is 0.2-0.4 mA of current, with respiratory arrest occurring at approximately 20-50 mA, and ventricular fibrillation at 60-120 mA2. Conducted electrical weapons typically deliver high voltages at relatively low currents.
When compared with other intermediate force options (such as hand-to-hand combat and chemical irritant sprays), conducted electrical weapons have the potential benefit of completely disabling a subject from a safe distance of 35 feet, without any short or long term medical consequences for the subject or the officer.

Are Tasers Safe?
The use of conducted electrical weapons has been associated with decreases in the use of lethal force against criminal suspects, as well as decreased injury rates among suspects and officers3,4. A recent review of 23 prospective human experimental studies found that a single exposure to conducted electrical weapons in healthy individuals is generally safe5. However, several case reports have called into question the safety of these devices, citing a temporal relationship between exposure and sudden death or dysrhythmia6-8. Importantly, these case reports have not proven causality, and are obscured by concomitant intoxication, medical comorbidities, excited delirium, or exposure to multiple shocks. Most recently, a case series by Zipes detailed 8 cases of Taser exposure associated with dysrhythmia or sudden cardiac death9. This article generated substantial interest within the lay press, as well as some controversy among the readership of Circulation10-13.
Other Taser-related injuries that have been cited in the literature include: intracranial penetration, ocular injury, pneumothorax, testicular torsion, pharyngeal perforation, and injuries associated with falls after Taser exposure5. Isolated cases of rhabdomyolysis have been reported in association with Taser exposure, but they are confounded by concomitant intoxication and agitation5. As with our patient, a theoretical risk to vascular structures remains plausible. However, there are no case reports of serious vascular injury in the literature, and the diameter of the barb is roughly equivalent to needles that are commonly used to obtain central access14.
Removal
To remove a Taser dart it is recommended that the surrounding skin be held taught and the dart removed with direct pressure. If the patient is unable to tolerate the procedure, injection of local anesthetic and use of a No.11 scalpel may assist the provider in cutting down to the barb tip for easy removal14. Notably, there is a groove along one side of the dart that correlates with the location of the barb tip. Advancing the barb forward through soft tissue (as is commonly done for large fishhook removal) is not necessary, owing to the small size of the barb and its linear shape. After removal, the wound should be cleaned and dressed in standard fashion. Sutures are unnecessary.

Case Resolution
The patient had a bedside ultrasound performed to more closely assess the potential for vascular injury prior to removal. Proximity to the internal jugular vein was noted. The barb was removed quickly with direct pressure. The patient tolerated the procedure well and was discharged to jail after having his wound cleaned and dressed.
Dr. Mike Miller is a 3rd year Resident at Denver Health Emergency Medicine Residency. Dr. Mandy Robar is an Ultrasound Fellow at Denver Health. Dr. Peter Pryor is an attending at Denver Health and Assistant Professor of EM at the University of Colorado School of Medicine.
References
1. Test results for the Model X26 conducted energy weapon (CEW) in accordance with TASER International device specifications. April 22, 2009. Report A85R9006/9031/9059B1.
2. Marx JA, Hockberger RS, Walls RM, Adams J, Rosen P. Rosen’s emergency medicine : concepts and clinical practice. 7th ed. Philadelphia: Mosby/Elsevier; 2010.
3. Jenkinson E, Neeson C, Bleetman A. The relative risk of police use-of-force options: evaluating the potential for deployment of electronic weaponry. Journal of clinical forensic medicine. 2006 Jul;13(5):229-41. PubMed PMID: 16442332.
4. MacDonald JM, Kaminski RJ, Smith MR. The effect of less-lethal weapons on injuries in police use-of-force events. American journal of public health. 2009 Dec;99(12):2268-74. PubMed PMID: 19846686. Pubmed Central PMCID: 2775771.
5. Pasquier M, Carron PN, Vallotton L, Yersin B. Electronic control device exposure: a review of morbidity and mortality. Ann Emerg Med. 2011 Aug;58(2):178-88. PubMed PMID: 21546120.
6. Strote J, Hutson HR. Taser safety remains unclear. Ann Emerg Med. 2008 Jul;52(1):84-5; author reply 5-6. PubMed PMID: 18565384.
7. Link MS, Estes NA, 3rd. Cardiac safety of electrical stun guns: letting science and reason advance the debate. Pacing and clinical electrophysiology : PACE. 2008 Apr;31(4):395-7. PubMed PMID: 18373756.
8. Justice NIo. Study of Deaths Following Electro Muscular Disruption: Interim Report. Washington, DC: US Dept of Justice, Office of Justice Programs, 2008.
9. Zipes DP. Sudden cardiac arrest and death following application of shocks from a TASER electronic control device. Circulation. 2012 May 22;125(20):2417-22. PubMed PMID: 22547671.
10. Heegaard WG, Halperin HR, Luceri R. Letter by Heegaard et al regarding article, “sudden cardiac arrest and death following application of shocks from a TASER electronic control device”. Circulation. 2013 Jan 1;127(1):e260. PubMed PMID: 23283865.
11. Ho JD, Dawes DM. Letter by Ho and Dawes regarding article, “sudden cardiac arrest and death following application of shocks from a TASER electronic control device”. Circulation. 2013 Jan 1;127(1):e259. PubMed PMID: 23283864.
12. Nanthakumar K, Waxman M. Letter by Nanthakumar and Waxman regarding article, “sudden cardiac arrest and death following application of shocks from a TASER electronic control device”. Circulation. 2013 Jan 1;127(1):e257. PubMed PMID: 23283862.
13. Vilke GM, Chan TC, Karch S. Letter by Vilke et al regarding article, “sudden cardiac arrest and death following application of shocks from a TASER electronic control device”. Circulation. 2013 Jan 1;127(1):e258. PubMed PMID: 23283863.
14. Roberts JR, Hedges JR, Chanmugam AS. Clinical procedures in emergency medicine. 4th ed. Philadelphia, PA: W.B. Saunders; 2004. xiv, 1486

2 Comments
What is the date of publication of this article?
I’m being electrically tased by my neighbors using radio frequency waves/signals to track and tase me. I can hear the high frequency sounds in my ear/head round about me. The longer they aim the more intense the pain that has lead to numbing of my hands/fingers. What doctor can detect such devices after affects?